TRENDS
5 Transformative Trends Shaping 3D Virtual Surgical Planning for Hospitals in 2026

In hospitals around the world, 3D technology has evolved far beyond just printing anatomical models. It's becoming a central component of the new standard of care, especially for complex cases. As adoption matures, surgical teams increasingly expect integrated workflows, smarter planning tools, and assurance around regulatory compliance. In this article, we share the five trends driving the next stage of growth for 3D planning and printing in healthcare.
1. From standalone 3D printing to comprehensive surgical planning
In the early days, many thought that 3D technology in surgical planning was limited to just 3D-printed anatomical models. Now, it's proven to be much more than that. What began as a groundbreaking innovation in select surgical departments has evolved into a routine, evidence-driven part of care, now implemented in more than 500 hospitals worldwide.
3D technology has matured into an integrated, everyday workflow that delivers consistent value for patients and clinicians alike. At the same time, the innovative spirit continues with extended reality (XR), artificial intelligence (AI), finite element modeling (FEA), and computational fluid dynamics (CFD), forming new possibilities in surgical planning.
Across hospitals, surgical teams are adopting a holistic planning approach that connects virtual 3D models, surgical simulation, XR visualization, and patient-specific device creation within a secure case management platform. They expect solutions that fit naturally into their clinical workflow, not standalone services. This evolution means providers must deliver interoperability, ease of use, and integration into hospital systems to support collaborative, evidence-based care from planning to surgery.
According to Radiologist Dr. Davide Curione at Bambino Gesù Children's Hospital, "3D planning for us in congenital heart disease has been a game-changer. It's helped us communicate with our colleagues. It's helped them realize what they have to do beforehand, to plan, to simulate. And, overall, I think this enhances the care that we give to our patients. It's made things smoother, better, and quicker."
2. XR gains traction as a powerful planning tool
In hospitals, XR is moving beyond pilot projects and finding solid ground in clinical practice. This is particularly true in fields such as congenital heart disease and oncology, where immersive, patient-specific visualization is becoming an invaluable aid in planning highly complex interventions.
Surgeons can explore anatomy in an interactive 3D environment, highlight challenges, and refine approaches before entering the OR. At Reina Sofía Hospital in Córdoba, Spain, the pediatric neurosurgery team combines virtual surgical 3D planning, 3D printing, and augmented reality (AR) to enter the OR fully prepared. They practice operations virtually with AR, planning each cut with precision.
This immersive visualization doesn't stop at the OR door, either. By viewing the preoperative plan in AR during the operation, the surgeon can compare actual bone cuts to the planned cuts and ensure precise alignment, making adjustments as needed.
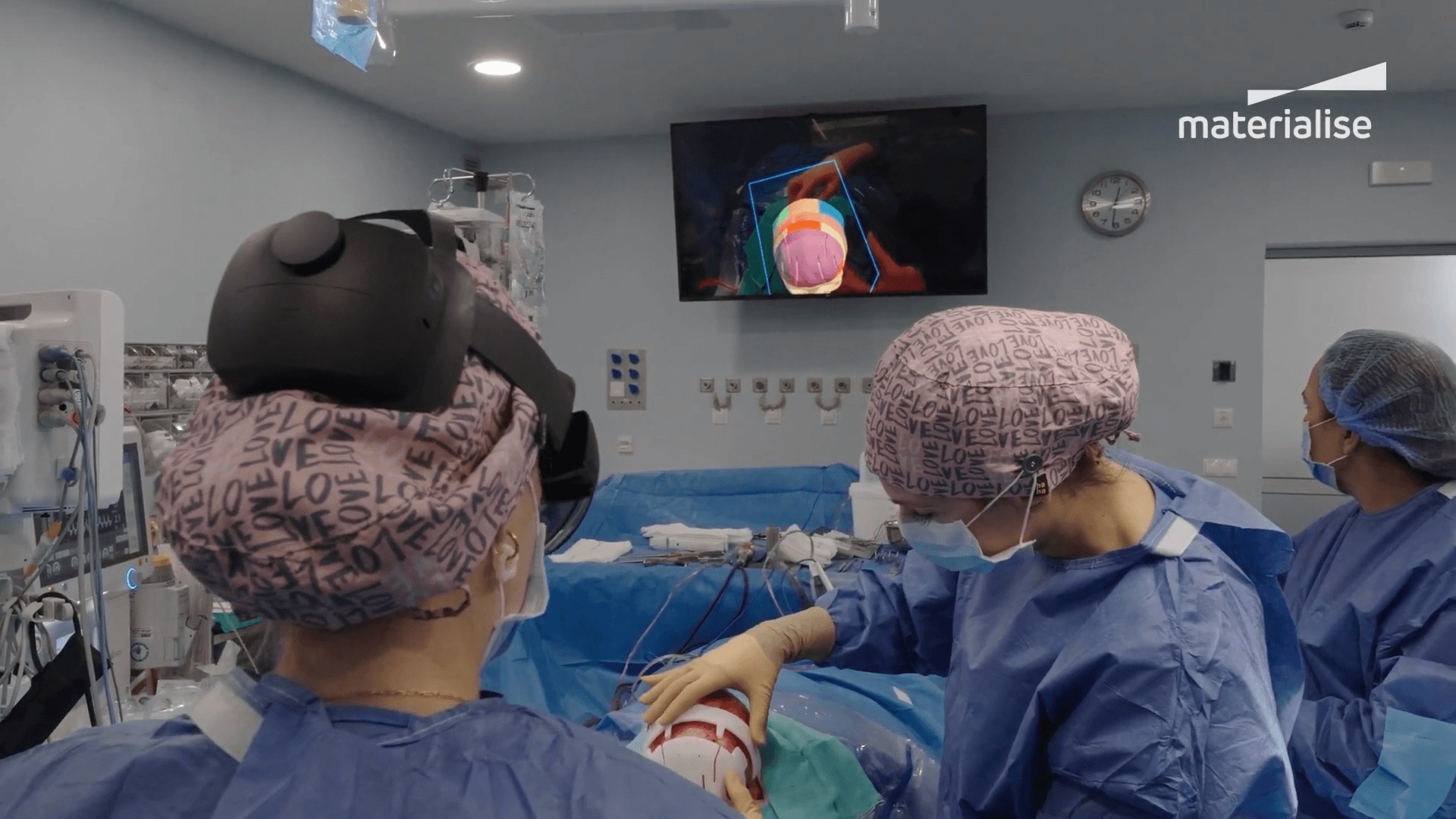
Taking it a step further, hospitals can connect XR to a regulatory-grade case management system for clarity and traceability. Every view, annotation, and decision is securely captured, supporting collaborative, evidence-based planning.
3. Case management becomes the strategic backbone of 3D planning
Another clear trend emerging in multidisciplinary surgical planning is the transition from ad hoc file handling to integrated case management platforms as the foundation of hospital workflows.
These platforms go beyond storing images and models; they provide governance, capturing who approved what, when, and for which patient. This ensures teamwide accountability, strengthens collaboration, and meets the growing regulatory demands for traceability.
This workflow became a turning point for collaboration at Radboud University Medical Center's 3D lab, helping the team scale up to 1,000 cases annually without sacrificing precision.
"In the past, we relied heavily on email threads and Excel spreadsheets, which led to inefficiencies and errors," shared Bas Kramer, a Technical Engineer at the lab. The online case management platform "provides structure, minimizes administrative burden, and improves traceability, which is crucial for meeting regulatory standards."
4. AI accelerates and simplifies 3D planning
Last year, we predicted that AI would drive market expansion. Since then, it's become even clearer that AI-enabled tools in 3D planning are moving from concept to everyday clinical use. Today, its most impactful application is automating anatomical segmentation, reducing the time needed for this process by up to 30%*.
By streamlining one of the most time intensive steps in the planning process, AI frees up time for healthcare professionals to focus on interpreting and refining the surgical plan. As algorithms are validated and integrated into regulatory grade workflows, AI's role will continue to expand while maintaining the transparency and reliability hospitals require.
5. A clear shift in perception: from 'good enough' to 'clinically essential'
Worldwide, perceptions of 3D planning are evolving. While many hospitals still rely on 3D volume rendering, an increasing number are discovering how interactive planning with high-fidelity surface modeling can significantly improve surgical accuracy and patient outcomes.
This shift is driven by growing awareness of the difference between basic anatomical visualization with 3D volume rendering and more precise planning with surface modeling — giving surgeons a more complete understanding of the anatomy before the first incision.
As more hospitals adopt advanced 3D modeling into routine workflows, they report better preparedness, more trust built with patients and their families, and enhanced levels of physician confidence. According to Dr. Christoph Happel, Senior Physician and Head of the Cardiac Catheterization Laboratory at Hannover Medical School, "A 3D model is so much more intuitive than 2D slices. Understanding is the first thing you need to provide proper treatment to your patient. Interactive 3D models give us that clarity instantly."


Advanced 3D planning for life-changing care
In 2026, advanced 3D planning won't be innovation for innovation's sake — it will continue to be the new standard of care. Hospitals that harness XR, AI, and integrated case management are delivering safer surgeries, stronger collaboration, and better outcomes. The future isn't about doing more; it's about doing it smarter. And it starts now.
*Based on an internal study
L-104956-01
Materialise medical device software may not be available in all markets because product availability is subject to the regulatory and/ or medical practices in individual markets. Please contact your Materialise representative if you have questions about the availability of Materialise medical device software in your area.
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
