CASE STUDY
Precision in Pediatrics: Predictable Cranial Vault Reconstruction with 3D Planning and Patient-Specific Guides
When it comes to delicate cases like craniosynostosis, every millimeter matters. In Córdoba, Spain, children who face complex cranial deformities can now benefit from a more predictable surgical approach. The pediatric cranio-maxillofacial department at Reina Sofía University Hospital is redefining cranial vault reconstruction (CVR) by combining virtual 3D planning with patient-specific surgical guides.
Industry
Cranio-maxillofacial surgery
Key solutions
- Virtual 3D surgical planning
- 3D-printed anatomical models
- Patient-specific cutting and positioning guides
- Augmented reality (AR)
The impact
- Predictable surgical execution
- Reduced intraoperative time and uncertainty
- Improved functional and aesthetic outcomes
The challenge
Complex pediatric cranial reconstruction
Cranial vault reconstruction is one of the most demanding procedures in pediatric surgery. Treating conditions such as scaphocephaly and trigonecephaly requires precise skull reshaping while accounting for ongoing growth and development.
Today, many surgical decisions are still made intraoperatively, placing pressure on the surgical team during already complex and time-sensitive procedures. Achieving consistent functional and aesthetic outcomes requires not only surgical expertise but also a high level of preparation and control.
At Reina Sofía University Hospital, surgeons recently faced this particular challenge in the case of a nearly two-year-old patient with scaphocephaly. The team sought a way to shift critical decision-making out of the operating room and into a structured, preoperative planning process.
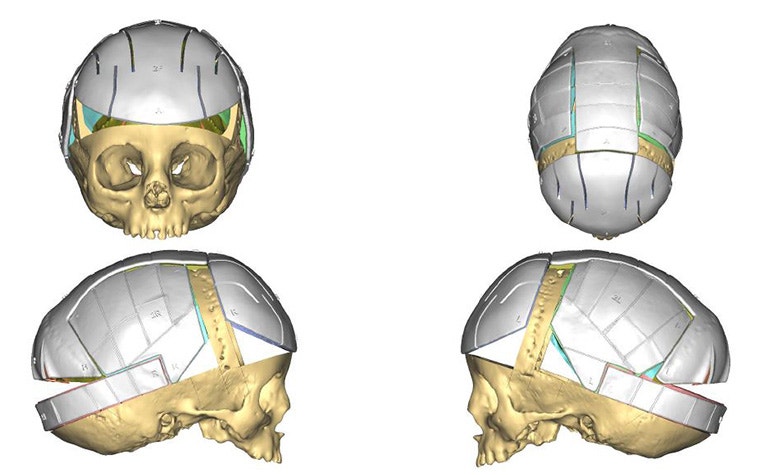
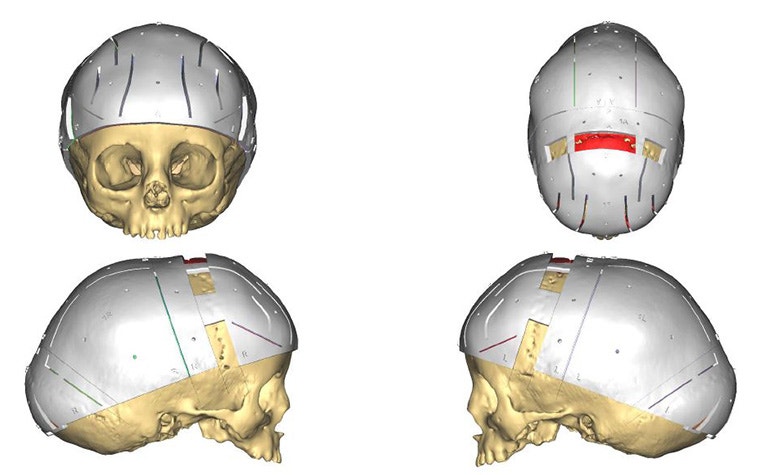
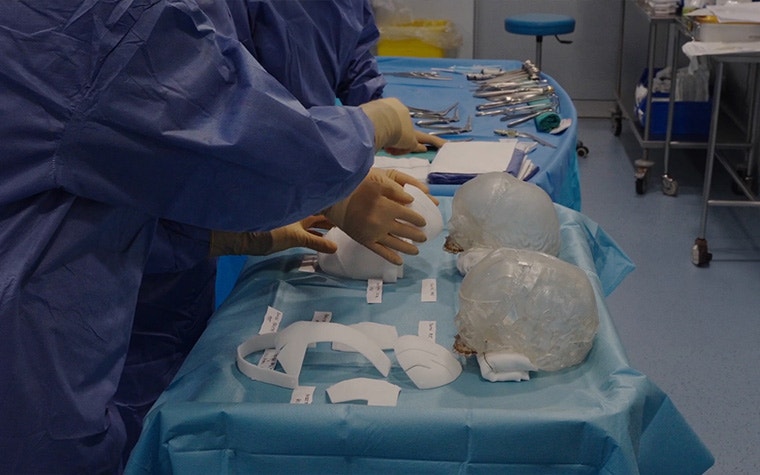
3D-printed positioning and cutting guides support the accurate transfer of the surgical plan to the OR.
The solution
From 3D plan to predictable execution
To address this challenge, the surgical team, led by Dr. Juana Vidal, collaborated closely with one of our clinical engineers to define a four-step approach.
1. Plan in 3D
To begin the surgical planning process, they translated MRI and CT data into a patient-specific 3D anatomical model. In this environment, the team can go beyond the limited visualization that 2D imaging provides. With the support of a clinical engineer, they segmented critical structures, including the sagittal and transverse sinuses, to plan osteotomies with complete awareness of anatomical risk zones.
Using patient-specific anatomical mirroring, they also determined the target cranial shape, balancing symmetry with intracranial volume based on the child's anatomy.
The team defined the osteotomies, bone repositioning, and final alignment step by step in 3D, creating a clear and structured surgical strategy before entering the OR. As Dr. Vidal puts it, "Virtual planning allows us to perform the surgery before the actual surgery." This level of detail allowed her to effectively rehearse the procedure in advance, reducing uncertainty and aligning the entire team around a precise, data-driven plan.
2. Prepare with physical models
Based on this virtual plan, they then produced a 3D-printed anatomical model. This physical copy provided an extra layer of insight into the patient's anatomy and a tangible way to validate their approach.
3. Execute with patient-specific guides
With a clear plan in place, the team needed a reliable way to transfer it into the operating room. That's where patient-specific cutting and positioning guides came in.
The guides defined exactly where and how the bone cuts should be made and supported precise repositioning according to the plan. Translating planning into execution in such a way reduces intraoperative variability and enables a controlled, step-by-step surgical workflow.

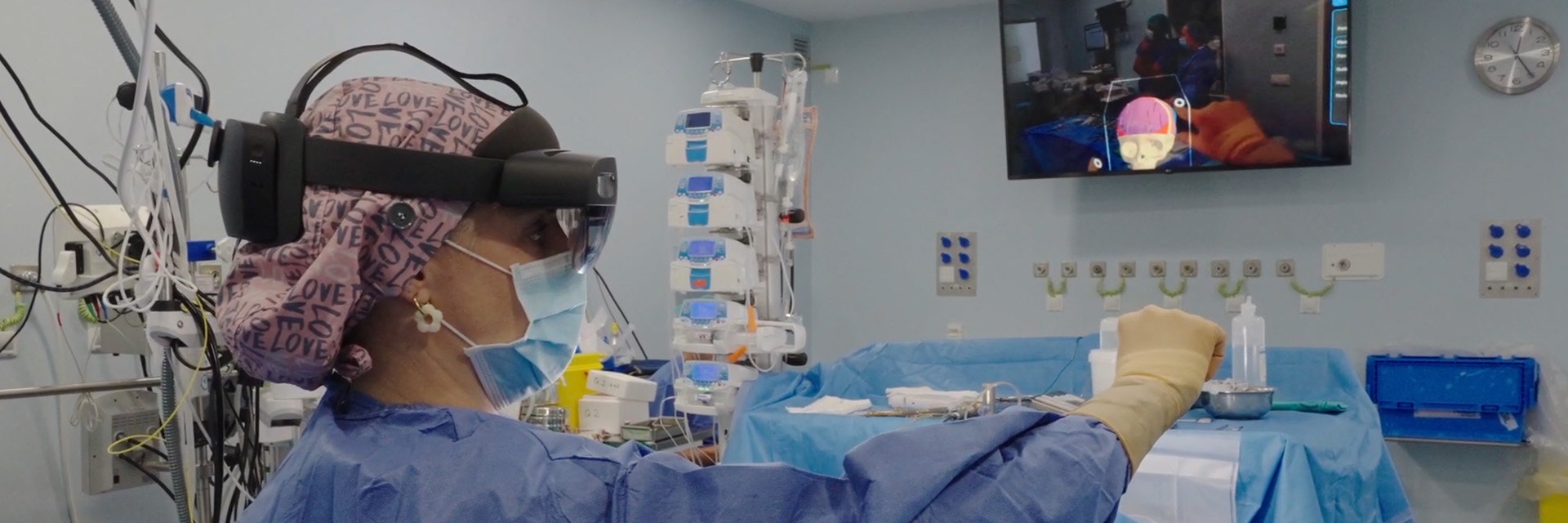
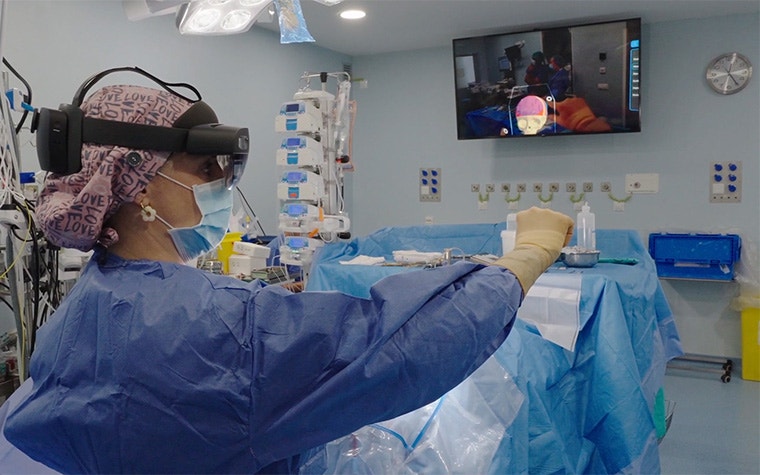
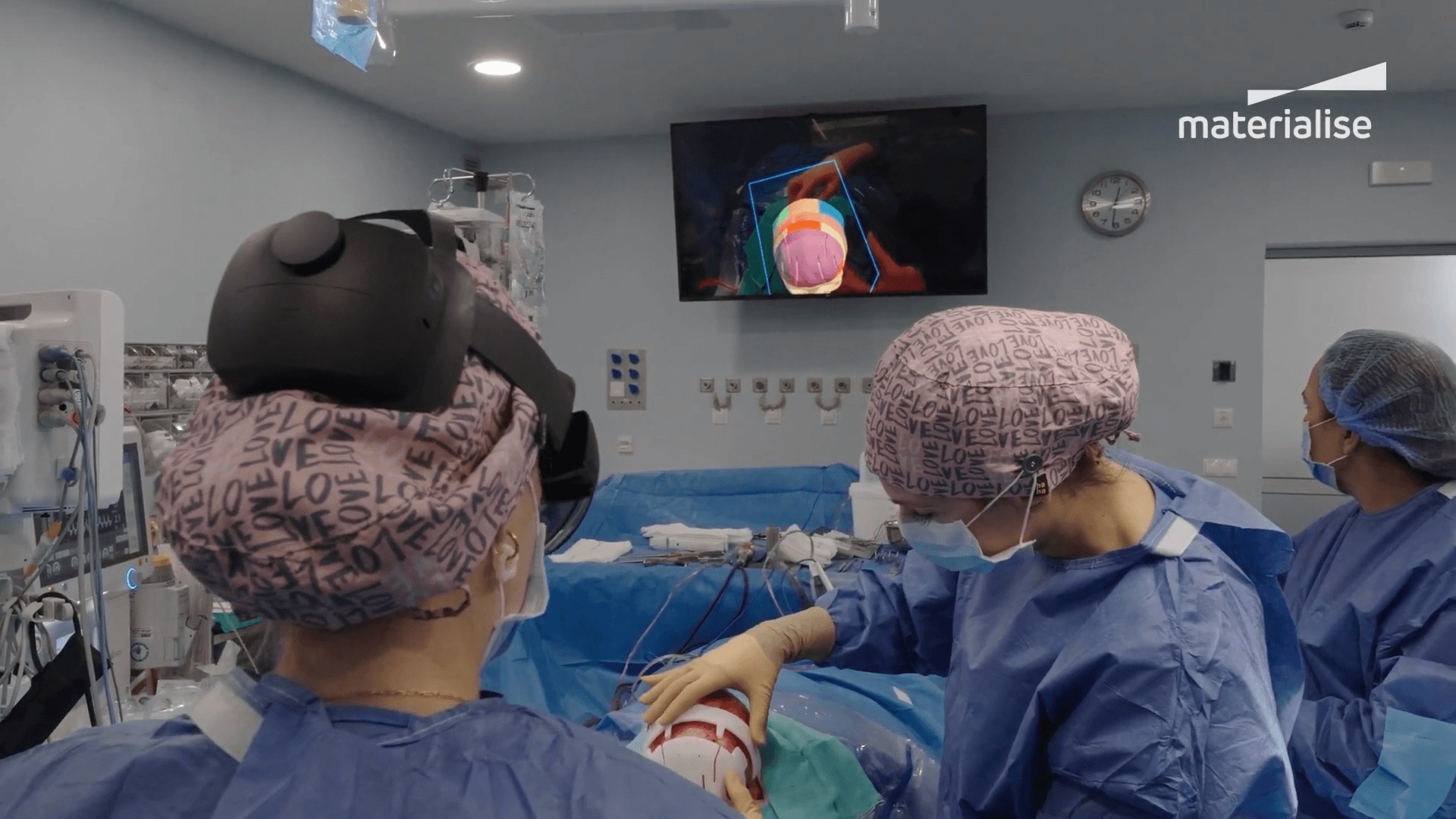
4. Immersive visualization with AR
As a final layer of support, the team used AR intraoperatively to compare actual bone cuts with the preoperative plan, validating alignment and positioning in real time.
The result
Efficiency, precision, and reduced risk
By defining osteotomies, repositioning, and cranial volume preoperatively — then transferring the plan through patient-specific guides — the surgical team achieved a more predictable and efficient procedure.
"Thanks to preoperative planning, operating room time is significantly reduced, which decreases the need for blood transfusions and enhances patient safety," says Neurosurgeon Dr. Marta Guzmán. "Moreover, aesthetic outcomes are more and more predictable and precise, increasing satisfaction for both families and the medical team."
Such a structured workflow helped reduce intraoperative uncertainty and let the team focus on execution rather than decision-making.
For this particular patient, the results have been very positive. The team achieved the planned volume and an excellent aesthetic and functional outcome in the shortest time possible. Now, the patient is in very good condition, with no complications from the surgery and good psychomotor development.
As this technology continues to evolve, surgeons will have an even greater level of confidence and control in cranial vault reconstruction. According to Dr. Juan Solivera, Head of the Neurosurgery Department, "This combination represents a major step forward toward more precise, safer, and patient-centered medicine, which is particularly important for pediatric patients with complex conditions."
Images provided by Reina Sofía University Hospital
L-104704-02
Materialise medical device software may not be available in all markets because product availability is subject to the regulatory and/ or medical practices in individual markets. Please contact your Materialise representative if you have questions about the availability of Materialise medical device software in your area.
Featured products and services
Share on: