EXPERT INSIGHT
Why Preoperative 3D Planning Tools Will Replace Conventional Imaging Tools
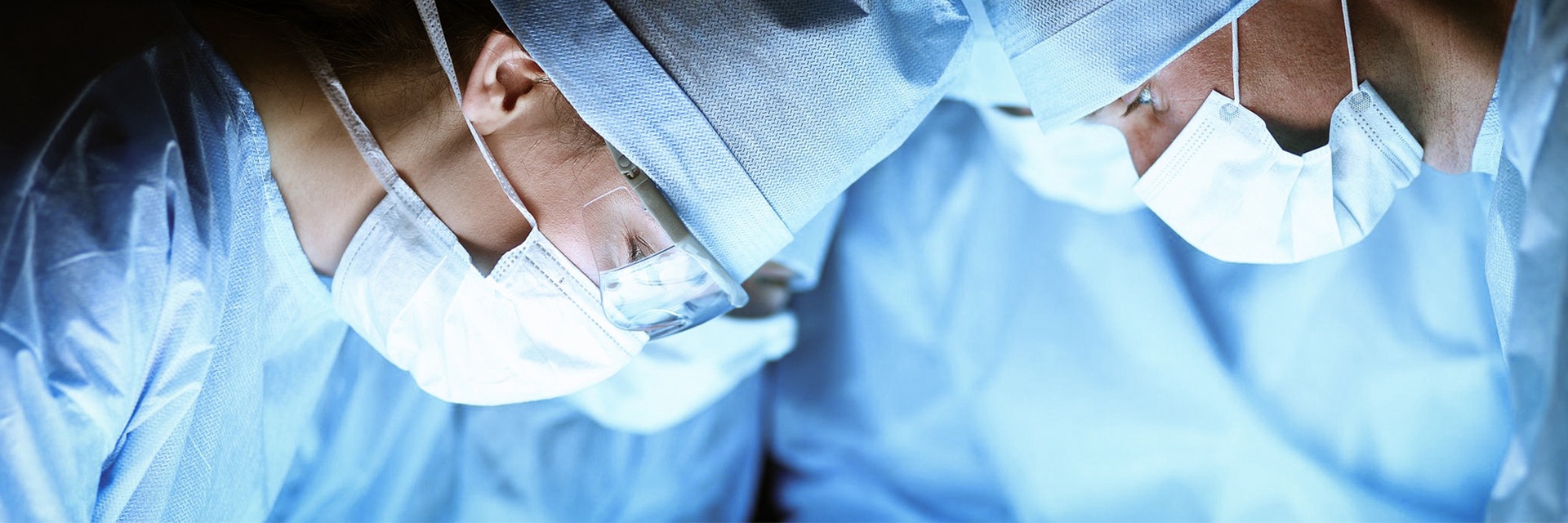
Orthopaedica Belgica hosted orthopaedic experts and 600+ participants at their yearly event in Brussels not so long ago. It featured an entire morning session on pre-operative templating in total shoulder arthroplasty. Here are highlights from presentations that were focused on 3D planning and personalized implants.
Olivier Verborgt
Preoperative 3D Planning, PSI, and Robotics in Shoulder Arthroplasty: Innovation and Evidence
3D preoperative planning and patient-specific instruments (PSI) are bringing new possibilities and proving very effective in shoulder surgery, shared Prof. Verborgt. With better designs and better results, surgeons are interested in taking on more difficult cases. Frankle MA, et al. performed a glenoid morphology using 3D analysis and discovered that 40% of glenoids that get reversed are deformed. With these kinds of challenges in glenoid cases, shoulder surgeons are looking to new technologies.
Most shoulder surgeons use a cannulated glenoid preparation technique for their surgeries. The successful correction of the deformity rests on the correct positioning of the central pin, which in turn, dictates the technique used for the surgery.


"3D preoperative planning is the new imaging tool. We can determine version, inclination, and medialization of the native glenoid in an accurate way,” Prof. Verborgt said. “Evidence of the technique’s accuracy is accumulating. It gives me the confidence that it works."
The question remains whether or not this technology is necessary in all cases. And although difficult cases are more interesting, it’s important to start with the easy ones. It’s a learning curve, said Prof. Verborgt.
Using the personalized guides is an advantage because you can execute precisely what you have planned.
Prof. Verborgt explained that the literature has shown that standard instrumentation is not very accurate if you compare it to PSI. His team did a preoperative study, looking at 11 patients with primary OA, an intact cuff but highly deformed glenoids. All patients underwent total shoulder arthroplasty (TSA), correcting the glenoid deformity using 3D planning technology. The results showed accurate corrections of the glenoid deformities, good stability, and low deviation from the planned position using an anatomical implant in all cases.
Preoperative planning and PSI are very helpful, but there’s still no evidence that this is the way to go, as long-term impact is still unknown. Is it worth the money? Is the clinical outcome better? How much can we correct? We still don’t know. But in regard to 3D planning, conventional imaging will disappear, and this will really be the future.
“We’ll use this as a planning tool on our smartphones. Templating helps a lot. It will make you think more about the surgery,” Prof. Verborgt explained. “It allows you to be more accurate; from 10% before, to 5% after the surgery. On CT images, it always looks worse than in 3D. I’ve been able to save a lot of patients from a reverse shoulder arthroplasty or complex bone grafting procedures using this technology.”
To the question “What percentage of good bone stock is enough to start?”, he replied: “In my opinion, if you have 80% coverage, it’s good enough. If it’s not possible, I would opt for an augmented baseplate, graft, or custom implant.”
For more data, please check the publication online: Accuracy of Patient-Specific Implantation of the Glenoid Component in Reversed Shoulder Arthroplasty.
Philippe Debeer
Reconstruction of Severe Glenoid Defects with a Custom-Made Personalized Glenoid Component
There are several treatments to choose from in challenging shoulder cases. Prof. Debeer discussed a system for the reconstruction of severe glenoid defects, the Materialise Glenius custom implant.
The process begins with the CT scan of the defect. Then comes the implant design, with adjusting the center of rotation and optimal positioning of the screws.
“The advantage of the Glenius system is that you can place the screws where most bone stock is situated. To aid in implantation of the prostheses and positioning and fixation of the screws, a personalized drill is also 3D printed,” Prof. Debeer said. “The tools and implant are produced following design approval, and an instruction booklet is included in the package.”


Prof. Debeer and his team conducted a study on 10 patients in which the new Glenius system was used. Five medical centers were involved. The clinical results were variable but with good pain relief, says Prof. Debeer, and all patients were satisfied. 80% of patients reported much better results than after their previous surgeries.
Only two complications were reported. Small differences were noticed between pre-op and post-operative positioning of the implant.
What does literature have to say about personalized glenoid components? Not that much, shared Prof. Debeer. He listed four articles he found online:
- Gunther MD, 2012: A polyethylene inset glenoid component was used. There was a good clinical outcome with significant mobility improvement. The problem with this implant, said Prof. Debeer, is that it’s not suitable for larger defects.
- Stoffelen, 2015: The case was of a total shoulder arthroplasty revision with a loose glenoid component. There were good results after 2 years.
- Chammaa (2017): 37 patients were evaluated for 5 years. There was a decrease in pain, but 16% revision rate.
- Ivan de Martino (April 2018): 2 cases with Zimmer Biomet component reported a satisfactory outcome.
The conclusion, according to Prof. Debeer, is that in selected cases with large glenoid defects, the Glenius solution is a good option. Short-term results are satisfactory, but we still need to wait for the long-term efficacy of the system, said Prof. Debeer, as well as for the result of bone ingrowth in the prosthesis. As for signs of radiographic loosening, Prof. Debeer said that his longest follow-up period was 4 ½ years after surgery, and there was no loosening whatsoever. Bone ingrowth was still uncertain, however.
A final question was brought up regarding the price and cost-effectiveness of the system. Although the cases they worked on were approved, said Prof. Debeer, cost remains a problem. And, as reimbursement will probably stop, the problem may increase.
Take a look at the clinical data summary for Glenius here.
Gert Van den Bogaert
Two-Stage Shoulder Revision with Personalized Glenoid Implant
There are four main causes of glenoid bone loss in revision, began Dr. Van Den Bogart. Subsidence, poly wear, metal wear, and infection. There are two current techniques to address these problems.
The first is bone grafting, which is difficult. In two recently published articles, the results showed that 1 out of 4 glenoid bone grafting had to be revised after 5 years. This method can lead to high revision rates, uncertain fixation, unpredictable offset, version, and inclination of the implant, and more.


The second technique is using off-the-shelf metal augment implants, more suitable for primary defects. However, this technique is also not optimal. The implant does not fit perfectly on defected area, and there is little control over the positioning of the implant itself and the screws.
Dr. Van den Bogaert then explained the two-stage revision with a personalized implant. The first stage begins with explantating the previous prosthesis, taking biopsies to check for infection, retaining the humeral stem and placing in a cemented spacer ball.
The team then performs a CT-based analysis of the glenoid defect, creates a personalized base plate, and plans the positioning of the screws. In the second stage of the surgery, which occurs approximately six weeks later, the implantation and fixation of the prosthesis occur. This entails the adaptation of the new glenoid sphere to the existing humeral stem or revising the stem.
Dr. Van den Bogaert talked about two cases in which this approach was applied and compared the results with those of existing techniques. Bone grafting fails to control offset, version, inclination, stability and ingrowth and standard metal augments do not fit the defect, he said.
He concluded that the new personalized implant fits the defect closely with correct native offset, version, and inclination. Inserting and fixing the screws more precisely allowed good stability.
Glenius is not commercially available in the US and Canada.
L-102924-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.