CUSTOMER STORY
Introducing 3D Planning to Interventional Cardiology: A Collaboration with the Henry Ford Health System
The Center for Structural Heart Disease at the Henry Ford Hospital under the leadership of Dr. William O’Neill is one of the leading structural heart programs. Dr. Dee Dee Wang, Director of Structural Heart Imaging at the Henry Ford Hospital and Medical Director of 3D Printing at the Henry Ford Innovations Institute, recently spoke at the Materialise World Summit. During her talk, she shared why 3D technology plays a critical role in their work on structural heart procedures and mostly transcatheter mitral valve replacement (TMVR) therapy.
Hope for high-risk patients
Henry Ford Hospital’s Center for Structural Heart Disease in collaboration with the Henry Ford Innovation Institute uses 3D and 4D imaging to enhance patient safety and procedural outcomes for high-risk structural heart interventions.The application of this novel technology allows Dr. O’Neill and his team to perform high-risk, minimally invasive TMVR on a more precise level for patients who have otherwise been turned down for traditional open-heart surgery. The team gives their patients hope and strives for patient safety.


The critical role of 3D planning
For Dr. Wang, the value of 3D technology is in the computer-aided design. She explains the two critical roles of 3D planning in TMVR interventions. One is to size the valve properly customized to each patient. The second is to make sure the depth and constraints of the valve fits in the patient’s heart without causing blockage of blood flow out the heart to the rest of the body (left ventricular outflow tract obstruction). Dr. Wang specifies, “Sizing is not enough with traditional CT. What we’re missing is computer-aided design. Because then you get technology to see depth, angulation, diameters, strength, constraints.”
Transcatheter mitral valve replacement is one of the high-risk structural interventions being performed in the world, with a high-stakes risk of potential for harm, even death, to the patient without adequate 3D planning. Dr. Wang explains, “Mitral valve disease is the number one valvular heart disease. It’s going to overcome aortic. However, it’s also the most high-risk procedure that can cause death at the table.” If a newly implanted valve blocks the passage of blood from the left ventricle to the aorta, patients can suffer life-threatening complications. Identification of risk of LVOT obstruction prior to the procedure in itself can prevent a complication and potentially save a life. This cannot be done accurately without 3D computer-aided design software modeling.
In addition, 3D technology and 3D planning make it possible for the team to test device sizes, catheters, and trajectories before approaching a case, says Dr. Wang. Providing a wider range of possible safety parameters gives the operators more confidence in handling high-risk cases.
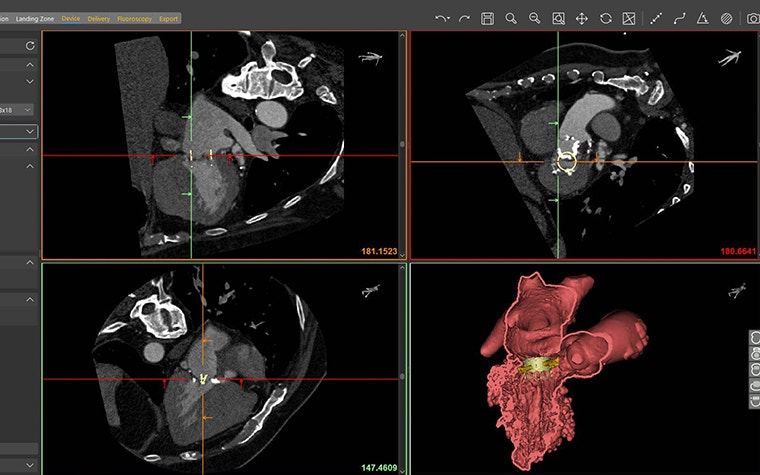

Mimics Enlight for TMVR
Mimics Enlight is based on the strengths of Materialise’s Mimics Innovation Suite (MIS), which has helped clinicians produce personalized 3D models for more than 20 years. The software was created in collaboration with Henry Ford Health System and Dr. Dee Dee Wang, and leverages the Henry Ford Innovation Institute’s patented workflow. Mimics Enlight supports patient selection and planning for structural heart and vascular therapy. It is the first of its kind to include consistent methods of taking critical measurements. This enables clinicians to reliably plan and screen patients for cardiovascular procedures.


Pioneering new methods for patient safety
During an interview with Materialise, Dr. Wang says that by using 3D planning, they can provide customized care to individuals with personalized and accurate 3D models using Mimics Innovation Suite and Mimics Enlight. This enables them to pursue their passion in pioneering new methods while exercising the utmost patient safety.
Mimics Enlight, with specific structural heart workflows, gives Dr. Wang accurate 3D models for consistency in taking measurements like neo-LVOT to screen patients for TMVR therapy, plan procedures, and determine the appropriate size and positioning of
TMVR devices. Dr. Wang explains their process, “In doing this we can model how and where we put the valve in our patient. So, while they’re at home watching their TV before they come to us, we take their CT scan, implant the valve at various positions, find out what valve size we’re going to use, and figure out what it’s going to be. We calculate the baseline LVOT surface area, what blood flow they live with. And then once we model a valve inside, we see what remainder of the LVOT they have left. And we can provide a cut-off.” The impact, she says, is a patient's life is saved.
L-101721-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
