CASE STUDY
Complex Glenoid Bone Loss Calls for a 3D Printing Solution
To successfully treat a patient suffering from complications after a total shoulder arthroplasty, Prof. Dr. Stefaan Nijs, Chairman of Trauma Surgery at Leuven University Hospital in Belgium, chose to work with Materialise experts and the 3D-printed personalized Glenius implant.
Industry
Healthcare
Key solutions
Glenius shoulder implant
The impact
Personalized solution
Preoperative planning
Higher accuracy and predictable patient outcomes
Addressing a complex defect in a TSA revision
Years after a total shoulder arthroplasty (TSA) on the left scapula, a 64-year-old male still had severe complaints. He suffered from a type 2 central defect with abnormal ossification surrounding the glenoid.
Prof. Stefaan Nijs, Chairman of Trauma Surgery at Leuven University Hospital in Belgium, took on the case and headed the revision surgery.
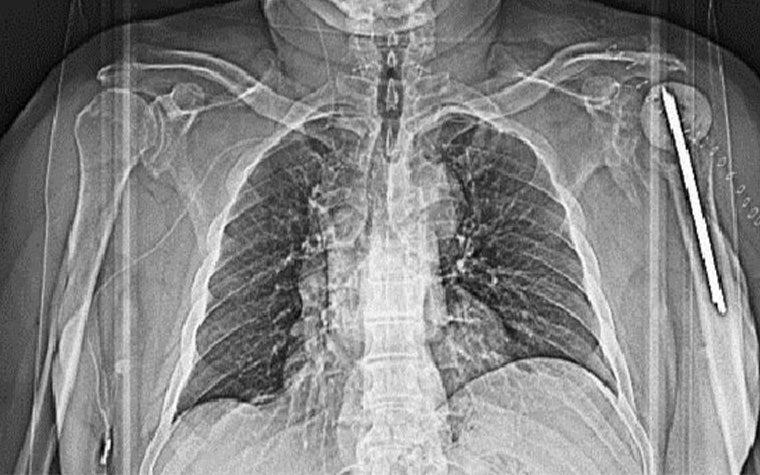

Left: Pre-op X-ray showing the old implant in the patient’s left shoulder. Right: Prof. Dr. Stefaan Nijs, Chairman of Trauma Surgery at Leuven University Hospital
Personalized vault loss reconstruction
Seeing the complexity and unusual size of the defect in the patient’s shoulder, Prof. Dr. Nijs chose to work with a personalized implant.
3D printing enables the creation of very specific and complex shapes and is, therefore, the optimal process for designing personalized components. Additionally, it facilitates the delicate construction of porous structures, an essential feature in the Glenius implant.
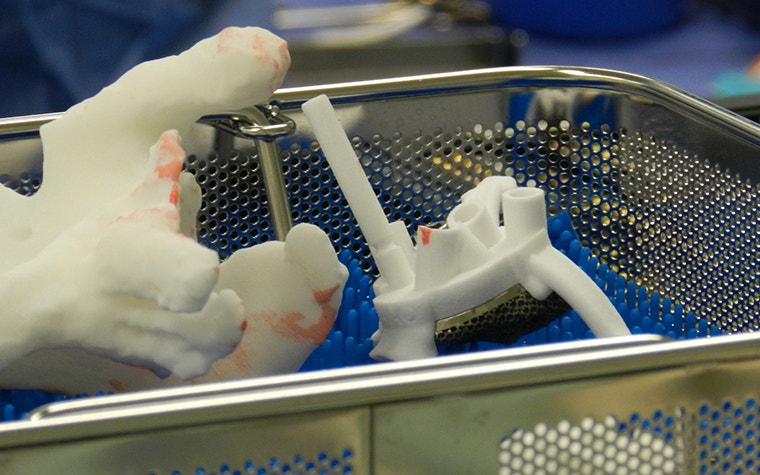
The plastic models and guides that were used during this surgery were printed with polyamide using selective laser sintering (SLS), and the metal implant was made using selective laser melting (SLM). DePuy Synthes Delta Xtend components were used for the humeral stem and liner.
Successful reverse shoulder replacement with a restored range of motion
In this case, Prof. Dr. Nijs performed a two-stage procedure. Stage one entailed removing the previous implant and inserting a spacer. In the second stage, the spacer was removed, and the Glenius was implanted.
The two-part surgery went smoothly and as planned. There were no incidents during the removal of the components. Removing the spacer, cleaning of the area, and tissue sampling for possible infection took roughly one hour, after which the surgical team was ready to place the implant. The insertion went very well, due to the welcoming size of the incision and the small size of the prosthesis.
Positioning and fixating the glenoid baseplate took approximately 20 minutes — 10 minutes less than expected.
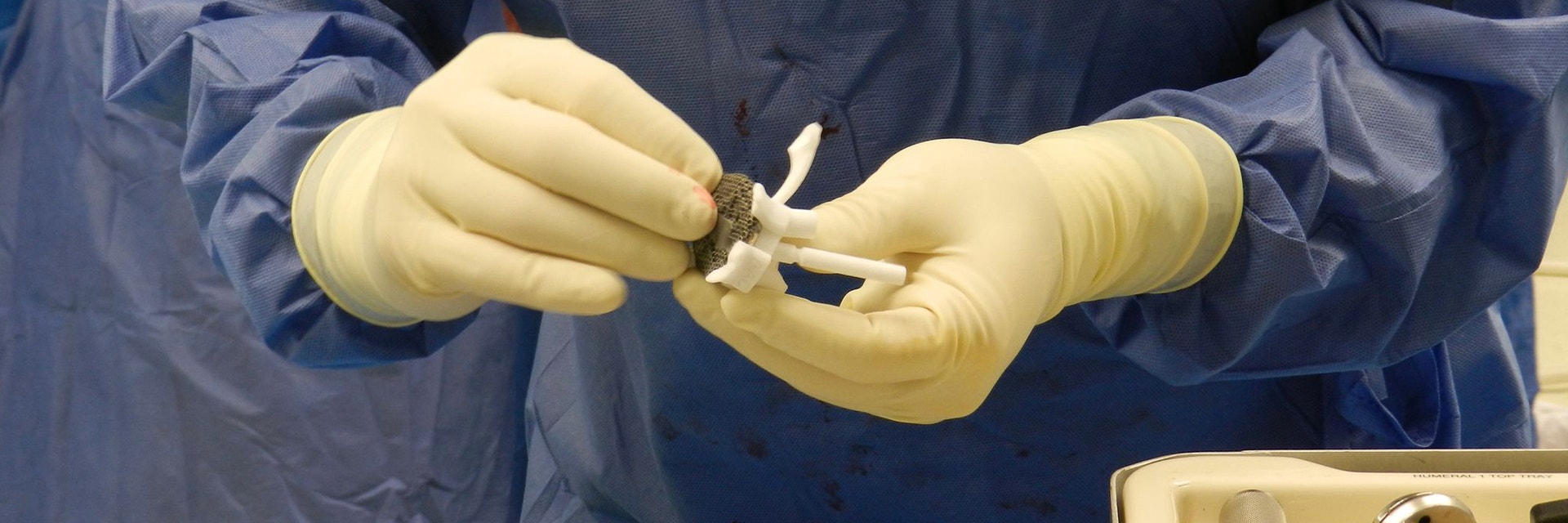
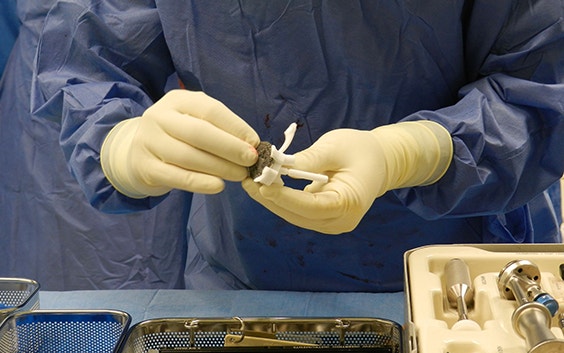
The surgical guides helped to find the unique position. Prof. Dr. Nijs first double-checked the position by testing the implant on the bone model. He then fitted the implant in its real position rather quickly, despite the smoothness of the defect surface.

Finally, he proceeded with the drilling, using the 3D-printed guide. The depth of the screw holes was verified before he inserted the screws. The first four screws fit as planned, but the fifth was more challenging due to no solid grip in the second cortex. However, as the length prediction of the previous screws was correct, Prof. Dr. Nijs continued with the planned screw length for screw 5.
Positioning and fixating the glenoid baseplate took approximately 20 minutes — 10 minutes less than expected. The surgical team removed the guide and proceeded with preparing the humerus for the sawing. A large part was removed to make the reduction easier. The team used a monoblock stem together with a 3 mm thin, high-mobility liner. After the trial reduction, the CoCr glenosphere was inserted. All components were in place after approximately two hours of surgery time.
Prof. Dr. Nijs was very pleased with the added value of the additional posterior support on the drilling guide, and with how smoothly the surgery went. The custom-made instruments that were designed for the glenoid implant made it possible for the trauma surgeon to accurately execute the preoperative 3D plan.
The postoperative report issued one and a half years after the procedure showed that the implant and screws were still in place. There are limited orientation and position differences between the analyzed planned position and the actual outcome.
So far, the surgery has prevented further revisions. Nearly two years following his second surgery, the patient is still happy. His shoulder’s range of motion has improved, and the patient has regained his independence.
Glenius is not commercially available in the US and Canada
L-102637-01
Featured products and services
Share on: