EXPERT INSIGHT
When Going Lean Means Changing Lives, Personalization Is the Key to Better Care
Improve quality, consistency, and efficiency while saving money. I know what you are thinking. I’m talking about going lean, right? Minimize waste; maximize productivity. The mantra of modern manufacturing.
Actually, yes, all of this, but applied to healthcare. It is not a surprise for those of us active in this industry that those manufacturing principles start to buzz around when most hospitals around the globe have challenging goals to improve patient care while maintaining profitability.
Different initiatives are being adopted across the global healthcare landscape, but I believe that the GIRFT program in the UK is an example to be mentioned.


The Getting It Right First Time initiative, or GIRFT as it is known, is a massive healthcare improvement program currently being rolled out across the UK’s National Health Service (NHS) — a program predicted to boost patient outcomes, support sustainable care, and potentially save the service around £1.5 billion per year.
GIRFT is all about best-practice processes and solutions that can truly improve outcomes for both patients and healthcare organizations.
And that’s great. Because it’s likely to mean that personalized patient care, a topic we are passionate about at Materialise, will also get in the spotlight. Not just in the UK. Worldwide. When going lean means changing lives, personalization may be the key to better care.
Why talk about GIRFT?
GIRFT was born from an initial study carried out by orthopaedic surgeon Professor Tim Briggs, which found that infection rates for patients in the UK recovering from hip and knee replacements varied from 0.2% to 4.5%. He questioned why and posited that if the procedures employed by the hospitals achieving 0.2% were followed by all providers, it could prevent a huge volume of infections and unnecessary treatment, including replacement operations, saving the NHS a substantial amount of money while simultaneously improving patient outcomes.
He had a point. Following the pilot, 70 hospital trusts reported savings of up to £30 million. Today, the GIRFT methodology is being rolled out across 40 surgical and medical workstreams across the NHS.
Frontline clinicians, experts in a particular medical specialty, visit health trusts to examine and discuss the challenges their peers face, procedures and processes they use, and the results they see. The idea is that best-practice care can then be identified and replicated system-wide, while unnecessary and unwarranted processes can be cut. Focus is firmly on solutions that deliver quality care and help reduce variations — variations being the range in approaches that led to the differences in infection rates I mentioned earlier.
Don't compromise. Personalize.
So, why focus on personalization when the objective is to eliminate variation in procedures and treatments? Wouldn’t a personalized approach mean more variation, not less, given that each case is in effect bespoke?
Quite the opposite. Because in this case, personalization becomes a consistent approach. The best-practice strategy for dealing with the reality that everybody is different. What works for one patient, particularly where surgery is concerned, often doesn’t work for another, even if they have the same root issue.
If we look at orthopaedic clinical reports, it’s been shown that around 15% of revisions in joint replacements fail — the failure rate for further revision being three times higher. Revisions based on a one-size-fits-all approach.
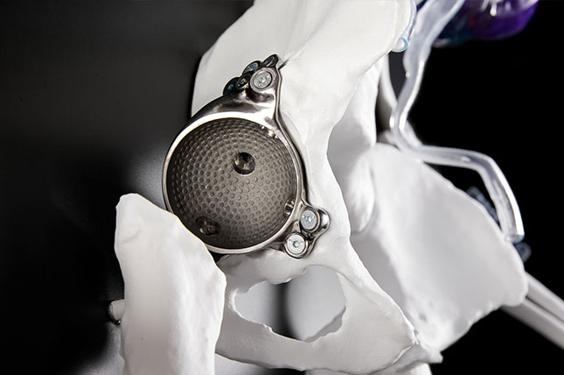

By contrast, take the example of our personalized aMace 3D-printed hip implant, which reports a 98% implant survival rate and 100% patient satisfaction.
Further studies from Bollard et al also report average cost savings per case of $1,488 and time savings of 23 minutes in the operating room when using 3D-printed surgical guides tailored to the patient.*
The advantages offered by surgical planning tools and personalized guides and implants are applicable to a vast variety of surgical treatments. And some of their benefits have already been raised by the GIRFT program.
Plan it right, predict it better... every time
With 3D visualizations and procedural and soft tissue simulations, surgical teams have a personalized blueprint for each surgery. They can predict what they will face in the OR and how best to approach it. And with 3D-printed guides, that plan can be actioned with improved precision…every time.
In fact, reduced time on the operating table was specifically highlighted in the GIRFT report on cranio-maxillofacial (CMF) surgery. Our experience in this field, particularly for 3D-printed surgical guides, even warranted Materialise a namecheck. As with orthopaedics, CMF teams are increasingly familiar with these techniques and the results they yield.


With current developments around AI, AR, and predictive modeling constantly enhancing the tools available, accuracy and predictability will only ever improve.
In the same vein, optimal planning and the tools used to achieve it inevitably help patients better understand their procedure and what outcome to expect — ensuring that expectations match reality. In 2017/2018, negligence claims against the NHS reached approximately £2.2 billion. While surgical errors will only account for a portion of this, the benefit of mitigating litigation risk cannot be overlooked.
Replicable, accessible, and achievable
Surgical planning and the use of personalized devices are replicable approaches that any hospital looking to achieve GIRFT objectives can successfully and sustainably adopt. 3D planning solutions are easily accessible, whether outsourced or produced in-house, with more and more hospitals utilizing software services to enable the production of visuals and printed tools at the point of care.
This is what going lean can mean for healthcare. With this in mind, I’m confident in, and excited about, a personalized future that benefits patient, doctor, health system, and society. And we at Materialise couldn’t be more committed to helping make it happen.
*Bollard et al., Medical 3D Printing Cost-Savings in Orthopedic and Maxillofacial Surgery, Science Direct, 2019.
Share on:

Meet the author
Brigitte de Vet-Veithen, Vice President, Materialise Medical
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.