EXPERT INSIGHT
How Accurate is Sizing Using Digital Templating for the Exeter Hip?
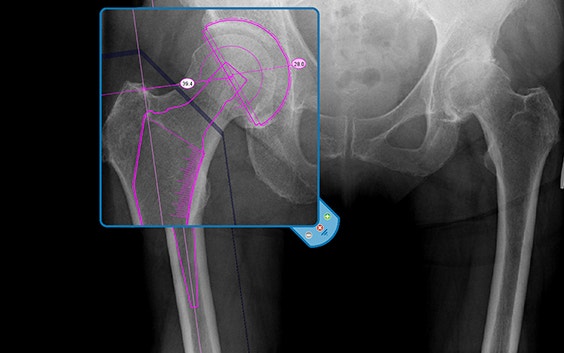
The following is a retrospective study of 39 consecutive primary Exeter total hip replacements (THR) carried out by Dr. Grant Shaw, orthopaedic surgeon in Portsmouth, UK to compare the Materialise OrthoView templated prosthesis size with the size used in surgery. The THR procedures were performed by Dr. Shaw between August 2016 and May 2017. Of the 39 procedures, 35 were elective hip arthroplasties and 4 were acute total hip replacements undertaken for neck of femur (NOF) fractures. All patients had standard AP pelvis for hip x-rays taken with a disc scaling marker placed in the hip plane.
Comparing the templated and actual results, Dr. Shaw’s study at Queen Alexandra Hospital in Portsmouth, shows an exact hip stem offset size match in 100%, an exact hip stem match in 85% and an exact acetabular size match in 87% of cases.
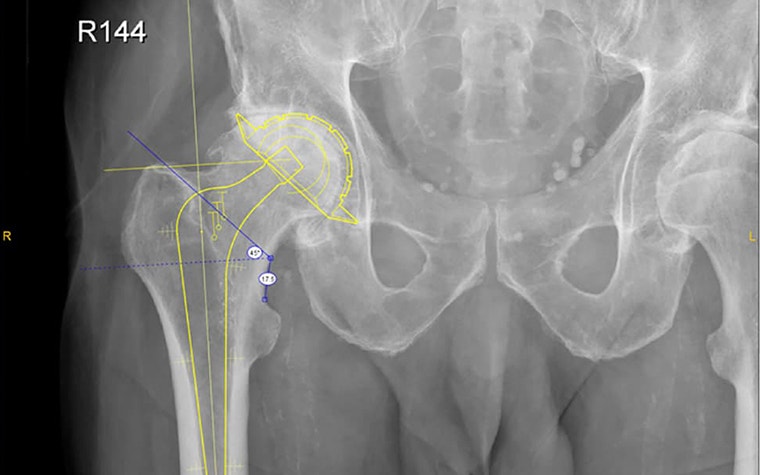

Dr. Shaw uses orthopaedic templates in all of his cases because he finds that “pre-operative planning of Primary THR using Materialise OrthoView on scaled x-rays is accurate and helpful.” In his conclusion, he identifies some of the key ways in which digital pre-operative planning helps him and his team to be better prepared for surgery.
Method
All the x-ray images were templated by Dr. Shaw using Materialise OrthoView Digital Pre-operative Planning Software. The resulting images and reports were saved back to the PACS and a copy of the templated sizes printed on what Dr. Shaw refers to as a “shopping list” or list of prostheses required. This list was used to collect the prostheses most likely to be needed for the surgery that day. In some cases, two optional sizes were recorded when the templating was between two sizes. A clinical decision was then taken at the time of surgery to identify the best option for the patient.
The component sizes recorded were stem size, stem offset, neck length for the 28 mm head, acetabular size and cement restrictor plug size. The neck length and plug sizes were roughly templated and usually two sizes were recorded on the shopping list because Dr. Shaw believes that these component sizes are best judged at the time of surgery.
The surgery was carried out through an anterolateral approach, Dr. Shaw’s standard technique. At the end of the procedure, the actual sizes were recorded on the Portsmouth arthroplasty database and the shopping lists were filed. All patients in the study received a cemented Exeter stem and a Marathon cemented acetabular component.
At the end of the study, an analysis was undertaken to compare the templated sizes with the actual prosthesis sizes used.
Results
Number of cases where two optional sizes were noted during templating for each component
Record of exact match between templating and actual component
Discussion
As in the table above, the templated Exeter hip stem offset matched the actual measurement in 100% of cases (all 39). Dr. Shaw commented that “in only 2 cases did I feel it necessary to hedge my bets by noting 2 possible sizes at the time of templating.”
The results also show that the Exeter hip stem size correlated exactly in 85% of cases, and in the other 15% the size used was 1 size different. Again only 2 cases had two options recorded from the templating. Of the 6 mismatches, 3 were oversized and 3 undersized.
Acetabular sizing was an exact match in 87% of cases, with 7 cases recording two options. All discrepancies were 1 size out. Of the 5 mismatches, 2 were undersized, and 3 oversized.
“Head length is regarded as a fine-tuning clinical decision taken at the time of surgery. For this reason little effort was made to predict the exact size at the time of templating and so two options were recorded from the templating in 41% of cases and a single option in 59%. These predictions were accurate in 92% of cases,” says Dr. Shaw.
Conclusion
Dr. Shaw uses pre-operative templating “primarily to predict component size”. The conclusion he draws from this study is “that templating proved to be accurate in between 85 and 100% of cases for all the hip components.” The mismatches were all within one size and equally split between over- and undersizing He adds that the size information resulting from a templated surgical plan “can be used during surgery in a number of helpful ways,” which he outlines below.
Prosthesis preparation
”The use of a ‘shopping list’ at the beginning of the day to move components from the theatre store into the operating theatre, saves valuable surgical time by having the correct components ready when they are required.” He continues, “it is also occasionally extremely helpful in alerting to a missing component at the beginning of the day, allowing time to rectify the problem.”
Scrub preparation
“Pre-op size anticipation is helpful for the scrub team as it can be used to predict the size of reamers, rasps and trials. This allows optimization of the instruments on the trolleys and is particularly helpful for junior and training staff who can be overwhelmed by the multitude of different sizes in the full set.”
Surgeon preparation
“I trust templating prediction of component size to be accurate,” states Dr. Shaw. “During surgery, if the surgeon finds a component size is different from the plan then careful examination for technical errors should be undertaken, rather than assuming the templating is wrong,” Dr. Shaw explains. “For example, under-reaming of the femur, resulting in an undersized and mal-positioned femoral component is quite a common technical error. This can be identified in this way and avoided.”
Finally, although Dr. Shaw believes that size prediction is the main advantage realised by orthopaedic templating software, he also identifies other benefits which are beyond the scope of his study. These include leg length correction, anticipation of issues with bone loss and planning to deal with a dysplastic acetabulum.
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.