EXPERT INSIGHT
Advantages of Using the S-Plate for Bilateral Sagittal Split Osteotomy
Recently, Professor Hervé Bénateau, with more than ten years of experience as the Head of the Cranio-Maxillofacial (CMF) Department at the Caen University Hospital in France and co-developer of the Materialise S-plate, conducted a webinar. In it, he shared his department’s clinical experience working with the S-plate to address a long-known problem in orthognathic surgery — managing the condylar position during bilateral sagittal split osteotomy (BSSO) without compromising on the occlusion.


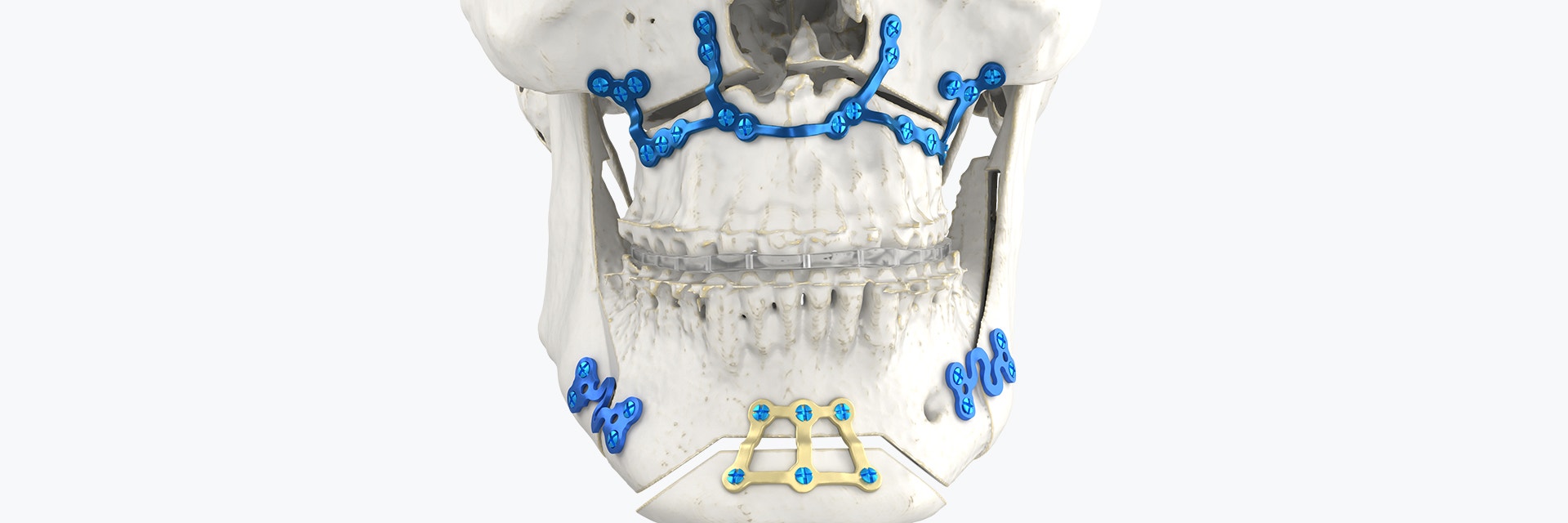
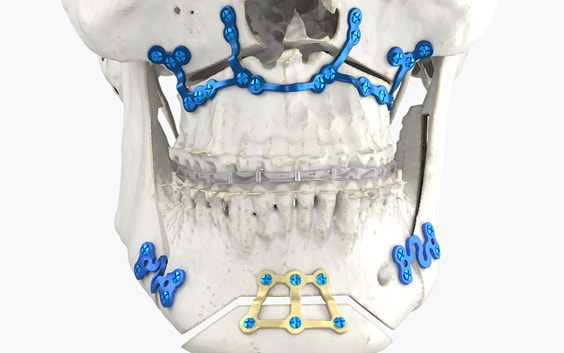
BSSO is one of the main orthognathic procedures used to manage skeletal mandibular excess, deficiency, or asymmetry and is known to be a technique-sensitive procedure. It can be used alone or in combination with a Le Fort I osteotomy for the maxilla. Here we outline the takeaways of the advantages that his team discovered.
Condylar positioning after BSSO is of utmost importance because it can affect post-operative skeletal stability. However, positioning the condyles is difficult as BSSO separates the mandible into three parts — the distal segment containing the dental alveolar region and the two proximal segments including the condyles. When performing a BSSO, the occlusion is first set in the desired position and then blocked temporarily by a maxillomandibular fixation (MMF) to control it. However, the MMF does not control the proximal segments with the condyles. They, therefore, have to be located manually by the surgeon before they can be reattached to the distal segment with osteosynthesis.
Obtaining the desired position of the condyles in their respective fossa, leading to a perfect occlusion at the release of the MMF, is an act of incredible precision. This requires a lot of experience.
Post-surgery
Several types of relapses can happen after osteosynthesis in orthognathic surgery. Immediate relapse is an unsatisfactory occlusion immediately at the release of the MMF when the condyles find their normal position, the so-called centric position. This is caused by a surgical mistake of inappropriately positioning the condyles in their respective fossa during the MMF. This can be uni- or bilateral and should not be neglected as this malocclusion can lead to long-term follow-up to TMJ pain, dysfunction, discomfort, and even to condylar remodeling or resorption. It is why it is so important to accurately control the position of the condyles relative to the occlusion intra-operatively during the BSSO.
Dealing with relapses
Several established methods have been developed to mitigate the difficulties. For example, some teams have developed surgical navigation to control the position of the condyles during the MMF. This has proven to be an accurate method1.
Another method developed has been the use of adjustable plates. They allow surgeons to adjust MMF. They can be based on plates with sliding systems or plates that can be deformed to adjust the position, such as the S-plate. The second group’s advantage is that the fixation of the osteosynthesis can be performed exactly the same as with a standard plate, but without the need to manipulate the screws again in case an adjustment is needed2.


S-plate specifics
The plate offers semi-rigid osteosynthesis, which can be defined as sufficiently rigid to obtain consolidation on the osteotomy site, but also with an increased flexibility to allow for some adaptation. In other words, it offers enough stability but avoids problems arising from absolute rigid fixation, such as pain or TMJ dysfunction. This semi-rigid fixation system can decrease the forces or the stress transmitted to the condyle in malpositioning to decrease the risk of long-term condylar resorption.
“Based on my experience as a CMF surgeon, using the S-plate is so easy that I believe it can improve the occlusal result in approximately 20% of the cases.”
— Professor Hervé Bénateau, Head of the Cranio-Maxillofacial Department, Caen University Hospital, France
Comparison to other adjustable plates
The S-plate has several advantages within the group of adjustable plates by deformation. First, due to its design, there is a smaller risk of breakage — it dilutes the deformation all along the plate. Secondly, it offers easier correction. Surgeons can act on the vertical plane depending on how they position the adjustment pliers. The possibility of the rotational movement it provides is of interest in terms of condylar positioning and the TMJ aspect.
With the S-plate, specific adjustment pliers allow the surgeon to obtain precisely what they want in terms of occlusion. As Prof. Bénateau mentions, “S-plates are very easy to use, and you can immediately see the result of their activation on the dental path (or occlusion).”
Adjustable or deformable plates can shorten the surgical time and allow the surgeon to work with more precision from the start. Additionally, it is a relatively simple procedure with an easy intraoperative correction of the occlusion. The operative time doesn’t increase and is shortened when occlusion has to be adjusted. All this at a reasonable cost.


Efficacy and long-term stability
Prof. Bénateau’s team performed a clinical study in their department to assess the true efficacy and long-term stability of using S-plates by examining post-operative cephalograms. These were taken on day one and at three and six months postoperatively. The data showed that there was perfect stability with the S-plate fixation3. Since then, he has performed several hundred BSSOs using the S-plate and has not witnessed any problems during his six-month follow-up with patients. Prof. Bénateau adds, “Based on my experience as a CMF surgeon, the use of the S-plate is so easy that I believe it can improve the occlusal result in approximately 20% of the cases.” He and his team will continue to collect data and look forward to helping more patients using the S-plate with proven long-term results.
L-102440-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.