EXPERT INSIGHT
The 3D Technology Behind NYU Langone’s Groundbreaking Double Hand and Face Transplant
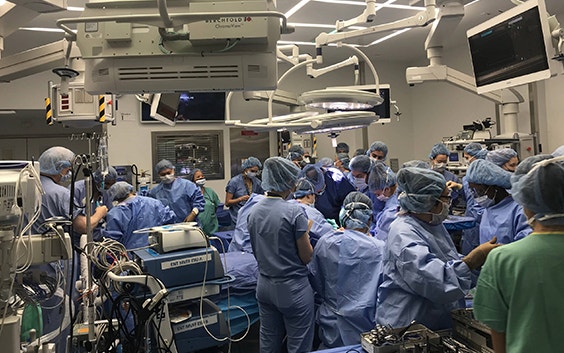
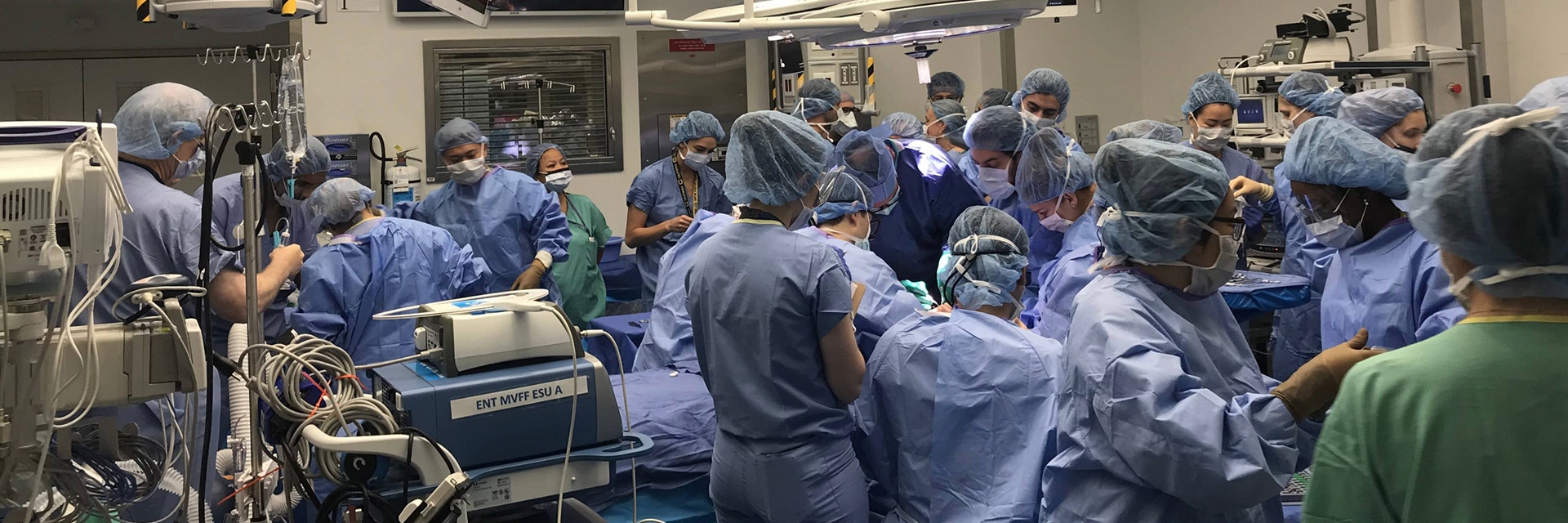
The double hand and face transplant, recently led by Dr. Eduardo D. Rodriguez at NYU Langone Health, is a testament to the value of 3D planning and printing for complex medical cases. The 3D technology revolutionizes the surgical process, starting with how clinicians communicate within their teams and with patients, to planning and performing surgeries.
Beyond the most complex cases, 3D technology is also increasingly used to deliver more personalized treatments for patients in everyday operations like jaw reconstruction or orthopaedic surgeries. With the addition of new technologies in the operating room, the surgical planning team is growing and changing to ensure they are used to their full potential.
A backstage pass to the operating room
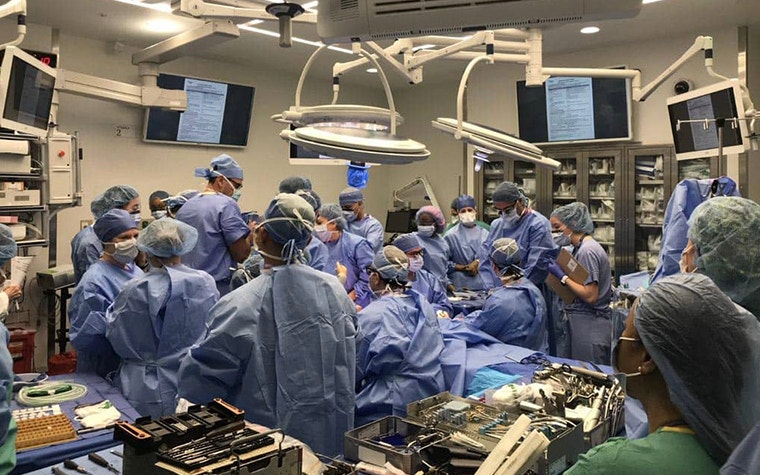

If you think of the operating room like a concert hall, the surgeons are the rock stars you see on stage. As with any major performance, the band is supported by other musicians and technical teams working backstage to ensure the show runs smoothly, managing the sound, visuals, and lighting.
In the operating room context, our team of clinical engineers (CLEs) plays this role, providing context and support in the surgical planning process. It all begins when we receive patient CT images and convert them into a computerized 3D model. We meet with surgeons to virtually plan their cases and provide engineering feedback to help solve their clinical challenges. With the help of our support teams, we provide the necessary input to design anatomical models, as well as personalized guides and implants.
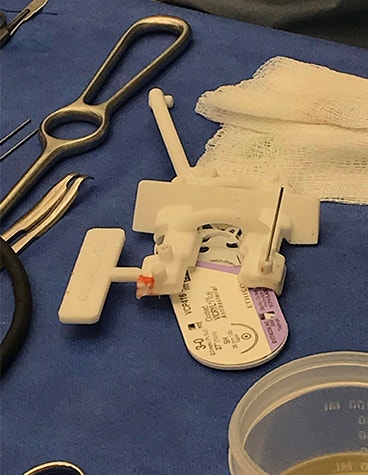
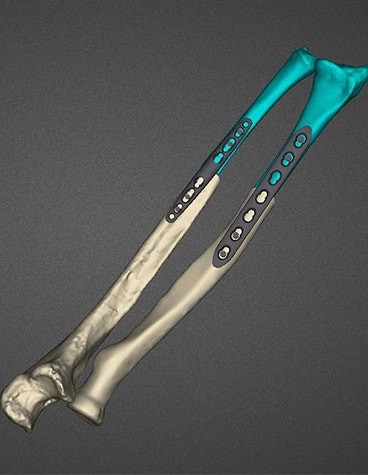
Planning and guides used for the hands transplant
Each of these tools serves a specific purpose in helping surgeons prepare and execute operations with greater confidence, efficiency, and precision in the OR:
- Anatomical models help surgeons better understand challenging anatomies and make the most suitable decisions before the surgery. When 3D printed, these models provide clinicians with a tangible representation of the patient’s anatomy. This is crucial to improving communication with patients and their families, but also valuable for educating residents and students on complex medical pathologies. Surgeons can also practice operations on these models and use them as a reference during surgery.
- Personalized surgical guides bring the benefits of digital planning to the actual operating room. They match the exact planned position and angle of interventions with the reality of the actual surgery. This can make surgeries quicker and possibly more cost-efficient by reducing the number of incisions and instruments needed.
- Personalized implants provide the enhanced predictability in surgical outcomes that surgeons need. With 3D-printed implants, clinicians can be confident that they will match the patient’s specific anatomy and needs, allowing them to concentrate on executing operations that can completely change a patient’s life.
The collaboration between CLEs and surgeons in surgical planning is relatively recent and has evolved with 3D planning technologies. Materialise is a pioneer in this field.
Our CLEs have unique expertise in 3D tools and technology capabilities, including how to implement them in the operating room. While you will not see us physically operating on patients, we are actively involved behind the scenes in every step of the surgical planning.
We provide recommendations on methods and best practices learned from our experience working on thousands of cases each year and collaborating with surgeons worldwide for different surgical needs.
The NYU Langone double hand and face transplant case clearly demonstrated the benefits CLEs bring to surgeons and patients. Materialise has a legacy of working in transplant cases, which demands a level of expertise not readily available in the market. What makes this case unique from our perspective is that, for the first time, our orthopaedics and cranio-maxillofacial teams worked side by side. Four Materialise CLEs were involved in this groundbreaking operation in the months leading up to this procedure, each of us focusing on our anatomical area of expertise. We worked alongside a surgical team of nearly 80 individuals to support 11 cadaver labs over 14 months. During each rehearsal, we worked closely with the six surgical teams involved, providing direction and making sure the 3D technology was developed and used in the best way to improve efficiency and accuracy in this time-critical surgery.
From a clinical engineering perspective, the biggest challenges in transplant cases are time constraints and variables in the donor’s specific anatomy. We can plan for the recipient’s anatomy, but each donor’s size and anatomy varies between lab sessions and the final operation.
In this time-critical case, our team designed and printed surgical guides and anatomical models for the hand transplant in different sizes to accommodate any donor that became available with minimal alteration. The 3D-printed guides allowed the pre-planned bone cuts to be replicated on both the recipient and donor to align the arms into the desired anatomical position for best results. They also guided the fixation of implants accurately for the best bone healing. Once a donor was identified, we finalized the cranio-maxillofacial (CMF) guides for the face transplant to match the donor.


In total, we 3D printed and delivered 180 parts for this case, based on CT scans of the donor and recipient. Two of our team members delivered the guides from our medical manufacturing facility in Michigan to the hospital in New York within 24 hours of receiving the final CT data. They were also present during the operation to address any technology-related questions during the surgery.
With the help of the detailed planning process and many rehearsals, the double hand and face transplant was successfully completed in 23 hours, shorter than Dr. Rodriguez’s previous face transplants that didn’t include the hands.
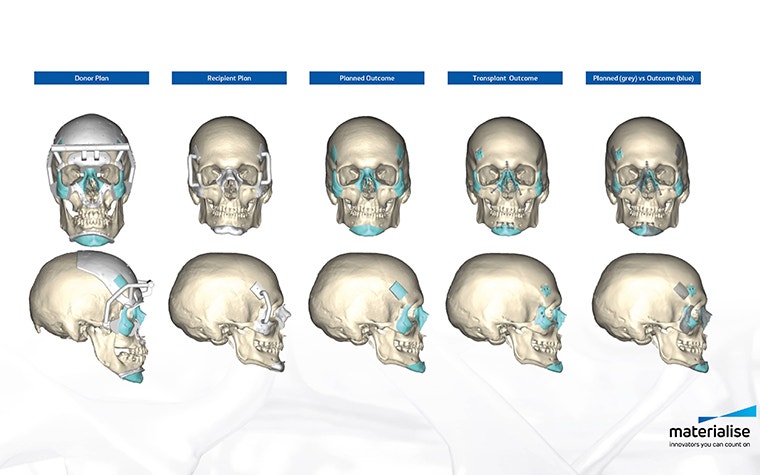

A fully guided system for bone fragment repositioning and fixation was unique to the patient’s anatomy and helped position the medical tools with great precision, reducing the overall surgery time.
3D tools for each step in the process
When approaching a new case, we provide input on the 3D tools and technology that would benefit the surgical team and their patients. 3D-printed personalized tools, such as the guides applied in the double hand and face transplant, are also increasingly common for routine surgeries. They provide surgeons with an additional level of confidence, resulting in improved patient outcomes. Personalized guides and implants are used in thousands of cases each year in knee, shoulder, and hip replacements as well as CMF reconstructions.
Surgical guides can improve efficiency in the OR by helping surgeons accurately position, cut, and drill through a guided system for repositioning and fixating bones. It can make surgeries quicker and possibly less invasive, reducing the number of incisions and instruments needed.
With implants created to match the patient’s anatomy, surgeons can maximize bone preservation by adapting implants to fit the patient, not the other way around.
The outcome: a better and healthier world
From our perspective as CLEs, the true value of this combination of technology and expertise becomes apparent when we see the direct impact of our work on patients’ lives.
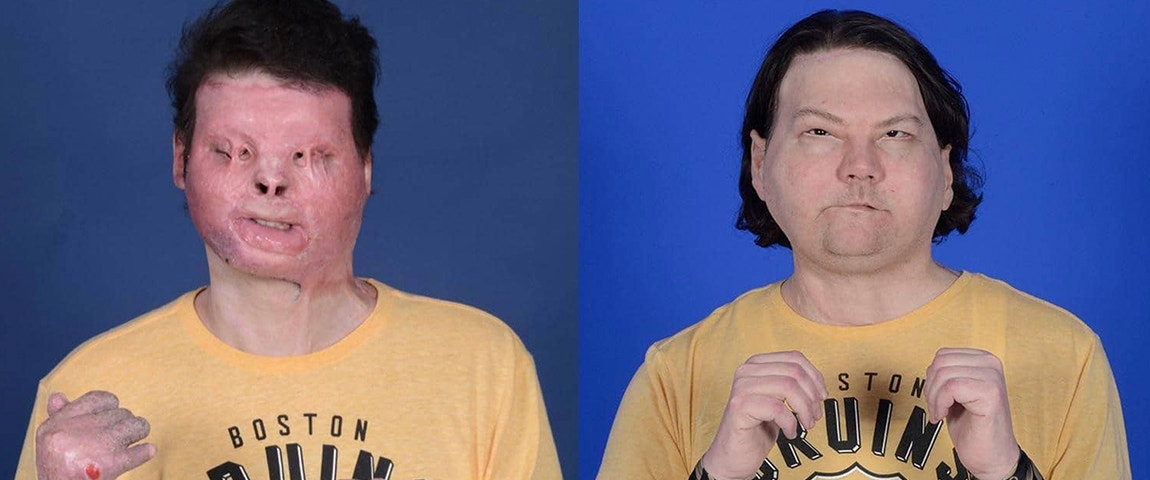
Joe DiMeo before and after the surgery. Image courtesy of NYU Langone.
When I saw the transplant recipient, Joe DiMeo, sharing his story at last month’s press conference, I was blown away by how well his recovery is going. Listening to Joe talking about how he got a second chance at life, it’s the greatest inspiration for the work we do as clinical engineers and an outstanding contribution to Materialise’s mission to create a better and healthier world.
L-101998-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.