CASE STUDY
Bespoke 3D Anatomical Modeling for 5-Year-Old Jalanea
When Jalanea was diagnosed with atlanto-axial instability — a dangerous point of weakness between the spine and skull — clinicians at Ochsner Hospital for Children in New Orleans used 3D anatomical modeling, generated by Materialise Mimics inPrint software, to help plan and successfully execute a complex, life-saving procedure in 2018.

Industry
Healthcare
Key solutions
Mimics inPrint
Point-of-care 3D printing
The impact
Preoperative planning
Enhanced patient communication
Higher accuracy and predictable patient outcome
The challenge
Plan and execute complex surgery to reduce atlanto-axial instability
Born with Down syndrome and undergoing treatment for leukemia, at just five years old Jalanea Lowe had already faced more challenges than most of us will in a lifetime. Yet a smile has never been far from her face. A huge personality and the support of an extraordinary family have given her a passion for life that is clear.
Jalanea’s challenges multiplied when she was diagnosed with atlanto-axial instability (AAI). AAI is a rare developmental anomaly, a weak point in the joint at the top of the spine/base of the skull that results in increased mobility around the cervical vertebrae.
For Jalanea, the condition meant it was proving increasingly difficult for her to hold up her head, making many everyday activities more and more impossible. She was having trouble walking and kept falling down. Worse still, the poor connection between skull and spine meant severe paralysis — even loss of life — was a real and imminent threat without immediate surgical intervention.


“To help Jalanea, the team needed to remove a small piece of bone located at this critical juncture, and use screws to stabilize the area in order to prevent damage to her spinal cord,” recalls Dr. Korak Sarkar, Neurologist and Director of Ochsner’s ‘m3D lab’ dedicated to leveraging new technologies that support state-of-the-art patient care, education, and clinical training.
A simple aim, but a highly complex and delicate procedure. Paralysis was a certain risk of inaction, but it could also be a potential outcome associated with the remedial action required.
The solution
Bespoke 3D anatomical modeling using Mimics inPrint
To fully understand Jalanea’s anatomy and meticulously plan the surgery, the Ochsner team turned to 3D printing and planning.
“For situations like this, 3D printing or ‘medical additive manufacturing’ is ideal and exactly why we work with partners like Materialise,” explains Dr. Sarkar. “X-rays, MRI images, and CT scans are invaluable for surgical teams in planning their approach and are typically used in conjunction with generic anatomical models to help map out the procedure well before a patient enters the operating room.
“3D anatomical models created from a patient’s medical imaging files, however, take this process to the next level by allowing surgeons to see exactly what they will encounter once a patient is on the operating table.”
“Being able to talk through the process with parents and do so holding a tangible model in your hands to clearly show the surgical steps ahead; that’s powerful.”
— Dr. Korak Sarkar
In-house capabilities at Ochsner Health System’s m3D lab enable the healthcare provider to print its own 3D anatomical models using techniques such as stereolithography and fused deposition modeling. But before any model can be created it must turn medical image data (DICOM files) into 3D print-compatible files. A task Ochsner trusts to Materialise’s medically certified and field-proven Mimics inPrint software in combination with an Ultimaker S5 printer.
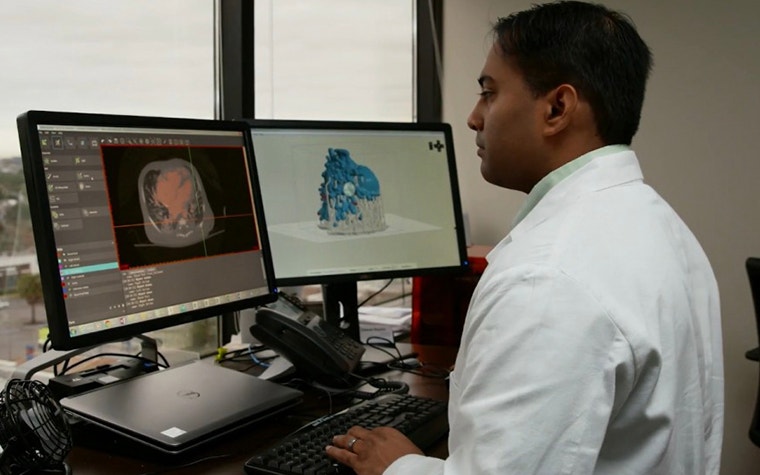

“In Jalanea’s case the Ochsner team had CT, MRI, and 3D echo imaging data as the starting point,” said Todd Pietila, Senior Biomedical Engineer and Business Developer at Materialise.
“These images were processed through inPrint’s segmentation and modeling algorithms to efficiently convert the DICOM information into 3D printable files with required supporting structures to ensure optimal printability of the anatomy. Finally, built-in verification functionality enabled the team to overlay the digital rendition of Jalanea’s model against the initial DICOM data to confirm accuracy and make final adjustments to ensure exact structural replication.”
It’s this level of verifiable accuracy that most appeals to Dr. Sarkar, and not just in terms of its value as a surgical planning aid.
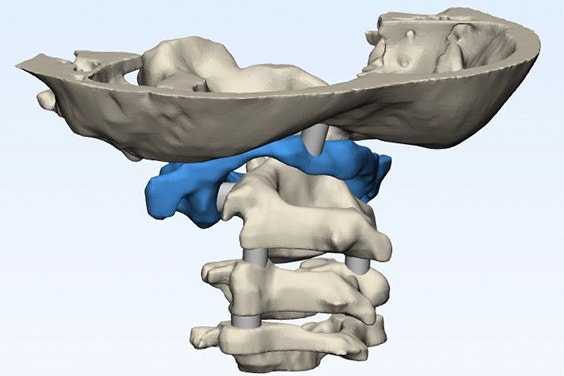

Render of the anatomical model of Jalanea’s spine and skull and Dr. Sarkar shows the 3D-printed model
“As clinicians, these tools enable us to see the exact task we will face. There is of course reassurance in that. But being able to talk through the process with parents and do so holding a tangible model in your hands to clearly show the surgical steps ahead; that’s powerful.
“When the team showed Jalanea and her parents the replica of her skeletal structure, they told us it gave them real peace of mind. Comfort. To help people feel that way, during what is an understandably traumatic time, is incredibly inspiring and rewarding. In fact, the family loved the model so much that they asked to keep it so that they could explain the process to others.”
The result
Meticulously planned surgery with an ideal outcome
Using the 3D model, Jalanea’s surgery was meticulously planned with all members of her clinical team clear on the specific techniques and steps required for her anatomy. The outcome was a surgical procedure that went exactly as intended. More importantly, a surgical procedure that has helped a five-year-old girl get one step closer to enjoying things she loved to do before the impact of AAI had made some of them impossible.
“Things could not have gone better in this case,” says Dr. Sarkar. “Jalanea has more battles to face but we all feel privileged to have played a part in helping her to get past at least one hurdle, empowering her to keep going and keep smiling. She was a perfect patient and using 3D printing was perfect for her.”
“For us, being able to bring [3D printing] expertise in-house means we can respond more quickly to cases like Jalanea’s and integrate this kind of ‘platform technology’ more deeply into our own existing processes.”
— Dr. Korak Sarkar
The 3D printing software used by Ochsner Health System integrates into the hospital’s clinical workflow, which means models are automatically numbered and logged against patient files for procedural safeguarding. All data used and the 3D printing files developed to create Jalanea’s spinal model will, therefore, become part of her ongoing patient record, providing a complete, data-rich audit trail of her treatment for future progress assessments and also to help plan any further procedures that may be required down the line.
Dr. Sarkar goes on to explain the value point-of-care 3D printing brings to his hospital: “Many hospitals outsource 3D anatomical model printing, which is great. But for us, being able to bring that expertise in-house — thanks to the functionality and process compatibility of the software we use — means we can respond more quickly to cases like Jalanea’s and integrate this kind of ‘platform technology’ more deeply into our own existing processes. Our aim is to use 21st-century technology to deliver 21st-century care. Working with Materialise has helped us with this mission.”
Materialise Mimics inPrint and compatible printers at the point of care
Point-of-care 3D printing is changing the way physicians interact with medical images. As diagnostic usage of 3D prints created at the point of care is increasing, scrutiny around the safe and effective use of this technology is required to provide healthcare providers with peace of mind. Materialise has the mission to provide products to the market that result in a better and healthier world, reflected in its ambition to create a safe environment to enable hospitals to 3D print at the point of care.
Increasing numbers of hospitals are turning to 3D printing of models as a tool to support complex cases, through multidisciplinary discussions and pre-surgical planning. The current method of choice for implementing 3D printing in hospitals is with a point-of-care 3D printing facility, leveraging in-house engineering and printing capabilities inside the institution.
L-100251-01
Share on:
