EXPERT INSIGHT
3 Perspectives on Pre-Clinical Virtual Testing and Finite Element Modeling in Arthroplasty
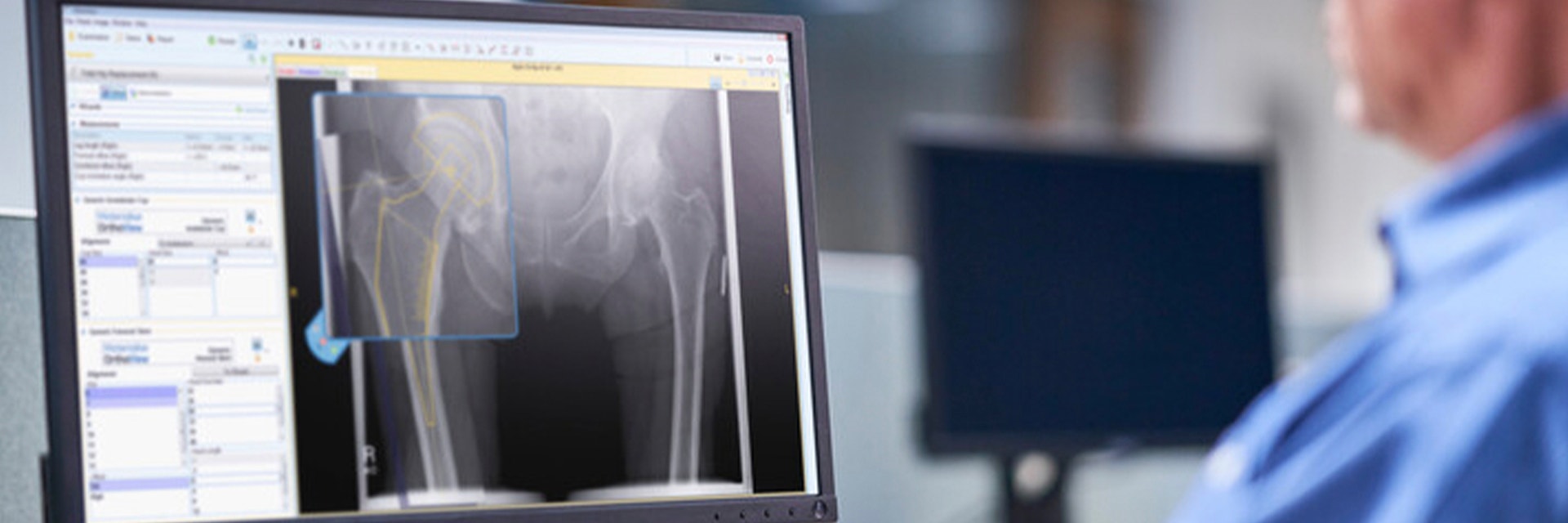
The International Society for Technology in Arthroplasty (ISTA) is one of the leading international conferences about innovation in orthopaedics. One of the best aspects of the conference is the mix of orthopaedic surgeons, academics, and representatives from the industry, who come together for fruitful discussions about new and ongoing topics in arthroplasty. We look back at the highlights and the insights we gained.
In the 'Computational Modeling in Arthroplasty' session at the conference, seven renowned speakers were invited to present their views on how modeling, if used in a sensible way, can help drive good decisions. The speakers discussed this topic from the viewpoint of an engineer, a surgeon, and a regulator.


Engineer’s perspective: choose appropriate failure criteria
There are still a number of challenges when it comes to finite element analysis (FEA) of bone-implant interactions from an engineer’s perspective. Constructing reliable models for individual patients requires specialized knowledge and still takes a lot of time. Therefore, it's important to streamline such processes. Furthermore, in the case of bone-implant interactions, not all constraints and material properties are known in detail, unlike that of a new car door design, for example. The old adage of “garbage in, garbage out” remains true. For example, it is important to choose the appropriate failure criteria for each particular situation (such as maximum values or peak stress). This ensures that the right boundary conditions are chosen and that the models are not overly complicated.


Surgeon’s perspective: challenge assumptions
Making sure the model was constructed correctly and challenging each of its fundamental assumptions are important from the surgeon’s perspective. For example, many of the first Charnley hip replacements led to hip fractures, which were initially difficult to predict with FEA models1. The reasons were not well understood until researchers realized that traditional elastic FEA models that did not allow for geometrical changes could be invalid. After all, when the surgeon hammers a femur stem into the femoral canal, the geometry of the trabecular bone is altered, which, as it turned out, was better captured with a model that had collapsible elements in it.
Regulator’s perspective: develop guidelines on computational models
From a regulator’s perspective, the FDA has traditionally been somewhat apprehensive when it comes to computational modeling as a supporting tool for new (510k) medical device applications. This perspective is changing. A steering committee with representatives from the FDA, clinicians, and the industry has been established. The committee is working on guidelines for the industry on how computational models can be used in support of new medical device applications. One key phrase in the guidelines will be “model credibility” (of which validation is only one aspect). Guidelines from both the FDA as well as the American Society of Mechanical Engineers (ASME) are expected to come out in 2018.


An aspect that arose several times was that most computational modeling studies still use only one or a few bones to perform virtual implantation and FEA modeling. The call for larger studies when doing pre-clinical testing for new implants or fixation methods echoed throughout the room, not just in this session but also in others.
As a believer of personalized computational modeling to improve patient care, Materialise allows more flexibility and automation in the software tools it provides to engineers and researchers. Through new scripting functionalities, users can now create their own workflows and make the link to finite element packages much easier. An example of how this is leading to new insights was shown in a joint presentation by KU Leuven and Materialise. In the study, KU Leuven investigated how a new calcar-guided short hip stem would perform in terms of stress shielding in a large population of femurs in an automated manner2. The study analyzed 96 femurs using the Scripting module in Materialise Mimics.
1 Should a Surgeon Trust the Model? Assessing the Clinical Relevance of Computational Models, Hirotaka Iguchi, ISTA 2017.
2 Effect of Anatomical Variation of the Proximal Femur on Stress Shielding Induced by a Calcar Guided Short Stem: An Automated Finite Element Analysis Study, Amelie Sas; Sjoerd Kolk; Pim Pellikaan; Thierry Scheerlinck; Harry Van Lenthe, ISTA 2017.
L-102652-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.