EXPERT INSIGHT
How Knee Guides Can Maximize Surgical Efficiency in Ambulatory Centers
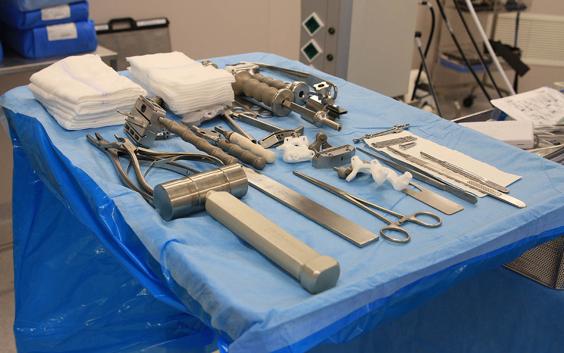
Hospitals and ambulatory surgery centers (ASCs) are under enormous pressure to balance costs while maintaining the best treatment for each patient. As knee patient numbers increase maximizing surgical efficiency may be the key to financial viability. Using the available operating theatres and hospital resources to treat as many patients as possible at an acceptable cost is a top priority for healthcare management. Personalized knee guides hold the potential to reduce costs and treat more patients in a single day without additionally burdening the hospital’s staff.
The shift of knee procedures from regular hospitals to ASCs has accelerated since Medicare and Medicaid changed the reimbursement landscape.
The number of hip and knee joint replacement surgeries performed in an outpatient setting is expected to grow by 73% from approximately 1.1 million today to about 1.9 million by 2026 (1.28 million knees + 620,000 hips)1,2.
Optimizing the total cost of treatment while keeping the same high-quality standard of care will be critical to enable this shift to ASCs further. Many ASCs find achieving this balance a challenge due to a lack of processes and tools that can help them increase efficiency.
Over the past ten years, 3D-printed surgical knee guides have been adopted by surgeons worldwide. Using personalized knee guides helps orthopaedic surgeons to transfer their pre-operative plan accurately and efficiently into the operating room (OR)3. The predictability that personalized guides enable help streamline the OR, reduce costs, and treat more patients in a single day.
Surgery time can be reduced by up to 13 minutes4 with knee guides when compared to using only conventional instruments.
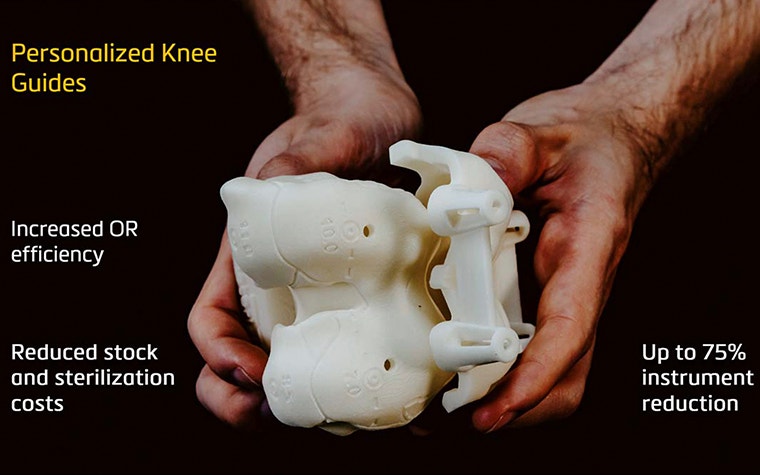
Up to 75% instrument reduction
3D preoperative planning and personalized guides significantly reduce the number of essential instruments required during surgery.
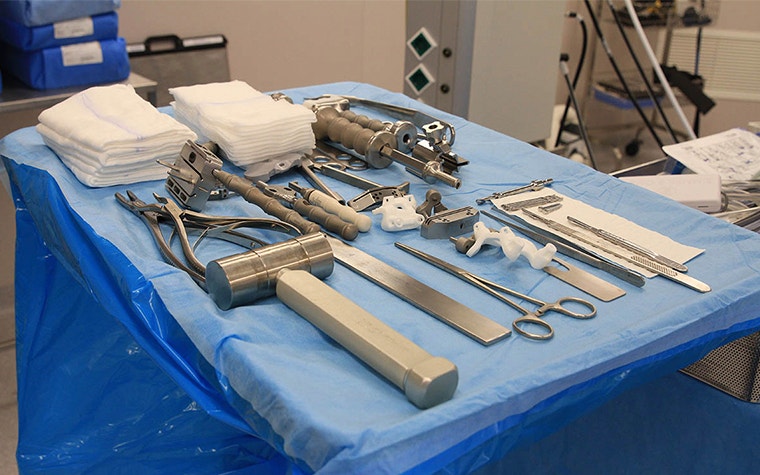

First, by knowing the size of the tibia and femur implants upfront, size-specific instrumentation and trial components can be reduced. Secondly, the traditional instruments necessary for alignment can be reduced to a minimum set, as the guides will accurately transfer the pre-operative plan and alignment into the OR.
When optimally streamlined, the potential gain can be up to a 75% reduction of instruments5 needed in the sterile field of the OR.
Reduced stock and sterilization costs
Reducing the number of surgical trays in the operating theatre also means reduced sterilization costs6. As less stock is required for each surgery, hospital stock and logistics can also be optimized, leading to cost savings.
Increased OR efficiency
This instrument optimization holds the potential to accelerate the OR set-up and turnover time. Additionally, this alleviates the workload for the circulating nurse and OR nurses , as they need to handle and carry less equipment.

Finally, the skin-to-skin operative time can be decreased thanks to fewer surgical steps. The surgery time can be reduced up to 13 minutes7, compared to surgeries using only conventional instruments.
As the list of ASC-qualified procedures expands and demographics increase, ambulatory surgical centers will treat more patients in the future. ASCs wishing to profit from this inflow must prepare now by reviewing current practices and streamlining procedures. 3D surgical planning and personalized guides are accessible technologies that ASCs should consider. These tools support ASCs tooptimize procedures while keeping the same high-quality standards .
L-101203-02
References
1 https://www.beckersasc.com/orthopedics-tjr/the-evolution-of-total-joint-replacements-from-the-hospital-to-the-surgery-center.html
2 https://orthopedicsc.com/news/ambulatory-surgery-centers-produce-successful-results-low-complications
3 Materialise Clinical Evaluation Report
4 Pietsch M., Djahani O.et al (2012) Custom-fit minimally invasive total knee arthroplasty: effect on blood loss and early clinical outcomes. Knee Surgery, Sports Traumatology, and Arthroscopy 36.
5 Depending on the instrument set used. Source: Zimmer Biomet
6 Noble JW., Moore CA. et al (2012) The Value Of Patient-Matched Instrumentation in Total Knee Arthroplasty. The Journal of Arthroplasty 27(1): 153-155
7 Pietsch M., Djahani O.et al (2012) Custom-fit minimally invasive total knee arthroplasty: effect on blood loss and early clinical outcomes. Knee Surgery, Sports Traumatology, and Arthroscopy 36.
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
