EXPERT INSIGHT
How Point-of-Care 3D Printing Was Implemented at Mayo Clinic
Jonathan M. Morris, M.D is a neuroradiologist at Mayo Clinic in Minnesota, U.S. and has been using 3D Printing for 16 years. The Mayo Clinic has three campuses in total and treats approximately 1,300,000 patients from 140 countries each year. Roughly 76,000 surgeries are performed in that same period.
At the Materialise World Summit 2017, Dr. Morris gave a breathtaking keynote presentation sharing the highlights of his knowledge. He captivated the audience with stories of his own experience with medical 3D printing and 3D visualization, and what's happened since the lab's implementation at Mayo Clinic over the previous ten years.
Starting with 3D anatomical models
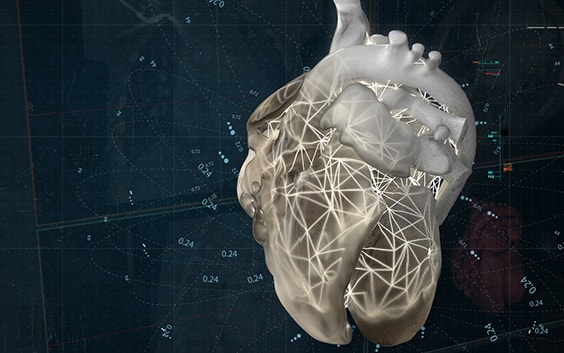
How did 3D printing come to be incorporated in a big organization such as Mayo Clinic? It had never been done before. Dr. Morris' team paved the way with a first, particular clinical case. A complex surgery on a set of conjoined twins with fused organs. The pediatric surgeons on the case requested a 3D model and Dr. Jane Matsumoto, who codirects the lab, was asked to get involved. Dr Matsumoto and Morris then worked together to build the clinical service needed.
After finishing the 3D anatomical model and handing it to the surgical team, Dr. Morris noticed something remarkable in the surgeons' way of working; something that was repeated with almost every model subsequently printed. There was more discussion surrounding the models and less around the images on the screen. It was a new and interactive way of examining the pathology in real, three-dimensional space.*
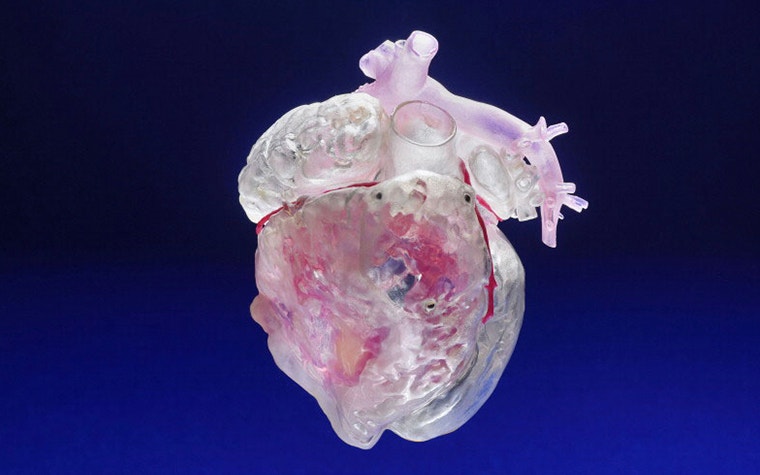

Making the unknown, known
Despite having access to a wide range of digital imagery X-Ray, CT scans, MRI, 3D CT scans surgeons are still aware that some things remain unknown until they step in the OR. "3D Printing bridges this gap of taking the unknown and making it known,” says Dr. Morris. 3D-printed models provide surgeons with a new way of visualizing the pathology, he stated. 3D-printed models allow surgeons to know things before they scrub in.
Tactics that paid off while setting up the 3D printing lab
Dr. Morris explained that transitioning medical 3D printing from a one or two use case scenario to a fully functioning clinical service that would serve the enterprise required planning. It entails the logistics of setting up an ordering system, workflow and a manufacturing infrastructure. The clinical team set up a validation workflow to ensure the printing quality. Challenges such as printing time, payment structure and materials are part of the equation and are improving.
Location is important too. "It has to happen where the doctors are," says Dr. Morris. The 3D printing lab should be located centrally. In their case, it was placed above the ORs. Once that was done, the 3D in-house lab took off, says Dr. Morris. The fact that it's in-house makes the lab very accessible for everyone, he continues. Surgeons can simply come by between surgeries, explain what they want to visualize, and leave the rest to the radiologists.
Dr. Morris found Materialise’s workshops helped to deepen Mayo Clinic expand their knowledge. “During the workshop at Materialise we had the chance to understand in depth the key aspects of additive manufacturing, in order to apply them to our company and reach our goals. It was a pleasure to see how a really innovative company works,” he said.


No limits
"Do not put up barriers to people using this technology because they'll use it in ways you can never imagine," says Dr. Morris. Let everyone access the technology with any request.
Surgeons often ask for things they don't know exist, and therefore don't have many technical limitations in what they're asking, says Dr. Morris. This has pushed the limits of what is being printed, in what material, color, and at which complexity level. The possibilities are endless - a complete face reconstruction, babies with severe skull deformities to oncological case, intracardiac anatomies, the possibilities are endless.
Teaching of the future
3D printing can bring medical education to the next level. 3D anatomical models can help medical students learn about rare abnormalities, for example. “Surgeons really want to be able to shorten the gap of their trainees to get from knowledge to experience. And 3D printing does that,” says Dr. Morris.
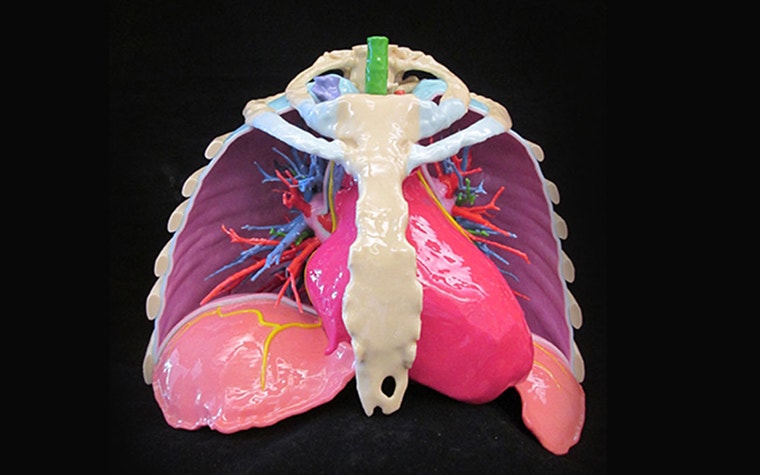
Dr. Morris wanted to print more realistic models, with real-life colors. One innovative way that he chose to use 3D Printing was by surface scanning a resected specimen of a tumor. In his presentation, he shows the 3D-printed model of the scanned specimen. This means that medical students can actually view what the pathology of a disease can look like. They can hold it in their hands instead of working with formalin fixed structures in jars. Since his presentation, champions such as Dr Maleszewski in the department of pathology have made this a routine process.

Want to learn something?
Watch Dr. Morris' keynote, and see some fantastic cases performed at Mayo Clinic, thanks to their in-house 3D lab. A mediastinal paraganglioma taken out through a keyhole, a severe case of Blount's disease. And a particular case of aortic aneurysm, Dr. Morris notes, in which the in-house 3D lab really proved crucial, a baby with his heart outside his body. Or are you curious about more common cases such as CMF tumors? Take your time and watch the video on the journey to your next convention. You won't regret it!
Materialise Mimics inPrint used in combination with validated 3D printers has been cleared by the FDA for the creation of anatomical models for diagnostic use.
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
