EXPERT INSIGHT
Knee Guides Precisely Execute Personalized TKA Alignment

In recent years, personalized alignment for total knee arthroplasty (TKA) has grown in popularity, intending to improve patient outcomes. At the same time, there is a growing consensus that precise enabling technologies are a necessity when choosing personalized alignment. In this article, we provide insights into the precision that personalized guides deliver as a cost-effective and easily accessible alternative to navigation or robotics.
Personalized knee alignment increases the need for precision
In the past few years, there has been an increased interest in alignment philosophies that are aimed at staying closer to the patient’s natural knee. Although, mechanical alignment (MA) is still the gold standard in TKA, this approach is often seen as one of the causes of patient dissatisfaction rates and residual symptoms because of its inability to replicate the anatomy and kinematics of a patient's natural knee.
Historically, procedures using alignment philosophies aimed to stay closer to the patient's natural knee have been challenging because conventional instruments for TKA are designed and developed to execute MA. The introduction of enabling technologies has significantly increased the ability of surgeons to use personalized alignment techniques.
While no conclusive clinical studies have demonstrated the superiority of one alignment approach over another, there is agreement that consistently reproducing a personalized alignment is difficult, and the use of enabling technologies, such as advanced imaging and 3D planning software, personalized guides, navigation, or robotics, is considered critical to its success )[1],[2],[3].
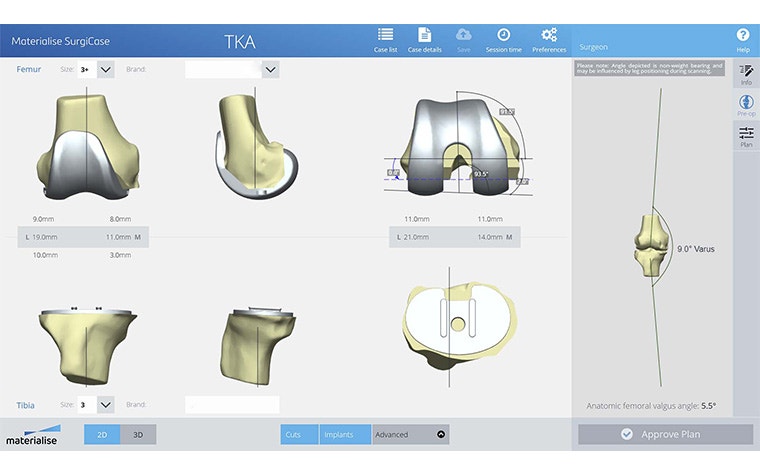

Enabling technology helps to achieve target alignment
Currently, there are no studies that have conclusively established a link between the use of technology and improved functional outcomes, and it is expected not to be demonstrated (yet) – as the output is highly dependent on the surgical plan the surgeon is aiming for with the procedure. Also, the optimal alignment for each patient is still a topic of debate.
However, several clinical studies describe the need for precisely executing any pre-operative plan. A network meta-analysis that included 90 randomized controlled trials, involving 9389 patients and 10,336 TKAs makes it clear that the precision and execution of new technologies is at the same level in terms of post-surgical outliers or patient outcomes, to the Knee Society Score or WOMAC score[4] .
“Results from a recent cadaver lab (performed due to a product update), clearly showcases how Materialise’s guides can precisely transfer any alignment technique into the OR.”
The missing link now are studies that combine the precision provided by new technologies with the most optimal alignment technique for each patient.
Personalized guides deliver state-of-the-art precision
Over ten years ago, Materialise’s surgical knee guides were introduced to the market, allowing surgeons to precisely transfer a 3D pre-operative plan into the OR. Since then, more than 300,000 patients have been treated with this technology, and more than 1200 clinical studies have accessed the precision of guides in transferring an optimized patient-specific surgical plan into the operating theatre.
Along with this consistent clinical evidence, results from a recent cadaver lab (performed due to a product update), clearly showcases how Materialise’s guides can precisely transfer any alignment technique into the OR. The study was conducted in 2019 on nine cadaveric specimens. Results have shown that planned resections can be precisely achieved.
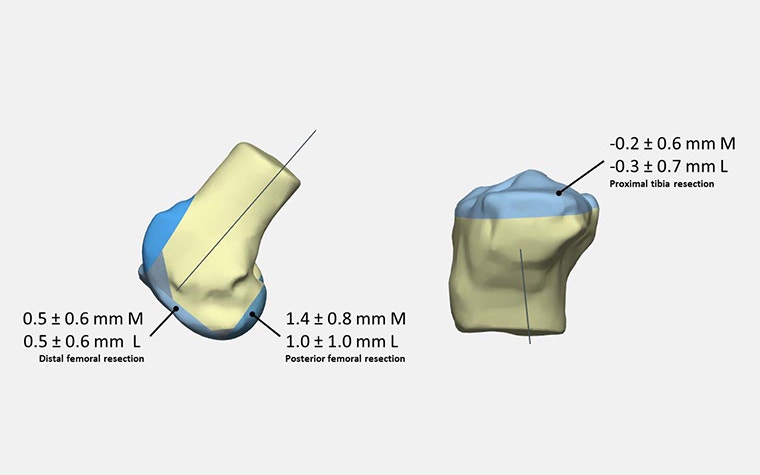

The image illustrates the post-operative accuracy of the femur distal, femur posterior, and tibia proximal resections for the nine specimens. Overall, the results are well within the acceptance criteria for accuracy in TKA: ±3 mm compared with pre-operative surgical planning.
A recent publication on robotically assisted TKA reports similar results from a cadaveric lab[5] . Using a similar approach in measurement, their results show that all resection mean differences were below 0.7 mm and standard deviations below 1.1 mm, which the authors report as similar in accuracy when using navigation.
A cost-effective enabling technology for personalized TKA
In summary, the use of enabling technologies could assist surgeons, exploring alternative alignment philosophies and, eventually, may lead to conclusions on the optimal alignment for each patient — further improving patient outcomes.
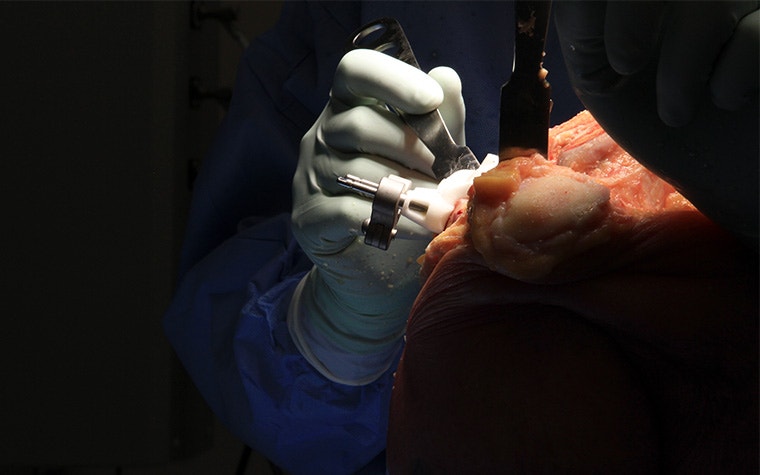

Today’s surgeons have a range of technologies that can help them to execute surgery with improved precision. Access to these technologies depends on the surgeon’s choice and hospital budget.
In combination with 3D pre-operative planning, personalized guides remain a cost-effective and easily accessible technology to any surgeon aiming to optimize TKA procedures with low initial investment costs.
[1] Goyal N, Patel AR, Yaffe MA, Luo MY, Stulberg SD. Does Implant Design Influence the Accuracy of Patient Specific Instrumentation in Total Knee Arthroplasty? J Arthroplasty. 2015;30(9):1526-30.
[2] Stronach BM, Pelt CE, Erickson J, Peters CL. Patient-specific total knee arthroplasty required frequent surgeon-directed changes. Clin Orthop Relat Res. 2013;471(1):169-74.
[3] Pietsch M, Djahani O, Hochegger M, Plattner F, Hofmann S. Patient-specific total knee arthroplasty: the importance of planning by the surgeon. Knee Surg Sports Traumatol Arthrosc. 2013;21(10):2220-6.
[4] Bouché PA, Corsia S, Dechartres A, Resche-Rigon M, Nizard R. Are There Differences in Accuracy or Outcomes Scores Among Navigated, Robotic, Patient-specific Instruments or Standard Cutting Guides in TKA? A Network Meta-analysis. Clin Orthop Relat Res. 2020;478(9):2105-16.5.
[5] Parratte S, Price AJ, Jeys LM, Jackson WF, Clarke HD. Accuracy of a New Robotically Assisted Technique for Total Knee Arthroplasty: A Cadaveric Study. J Arthroplasty. 2019;34(11):2799-2803. doi:10.1016/j.arth.2019.06.040
L-102302-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
