
INTERVIEW
The Evolution of Personalized CMF Solutions for More Accurate Surgical Interventions
We spoke to Prof. Thomas Schouman, a cranio-maxillofacial (CMF) surgeon working at APHP-Pitié-Salpêtrière Hospital at Sorbonne University in Paris, about his invaluable experience being in the spotlight for personalized CMF solutions for more than ten years. Prof. Schouman is a European reference in CMF surgeries, and he was one of the first surgeons in the world to use personalized solutions in clinical settings. In this interview, he goes back in time to tell us how the development and adoption of those devices have increased accuracy in CMF surgeries.


You have been at the forefront of personalized CMF solutions for more than a decade now — when and how did you get involved in the development of these devices?
My involvement with personalized solutions goes back to 2005, when I started also working as a research associate in the biomechanics department. Back then, most CMF devices were almost hand-made, with a demand to enhance surgical tools. We saw the potential of personalized solutions to enhance surgical predictability, and therefore we initiated a collaboration with OBL, which is now the French part of Materialise, to develop those devices.
The fibula cutting guides used in reconstruction became our first collaboration with Materialise. Surgeons know how difficult it can be to shape a fibula flap. In 2009, we had our first surgery using the personalized cutting guides for fibula flaps in reconstruction.
This early experience was very interesting in terms of accuracy — we were so convinced about the added value of the cutting guides that we decided to use them on as many cases as possible. We were enthusiastic with the results.
How has the technology evolved since then?
As I mentioned before, in 2009, we started using personalized solutions in clinical routines with the introduction of the fibula guides. At the same time, Materialise developed a 3D-printed titanium implant with an innovative porous structure, and this was a huge step in the CMF market. For the first time, we could have personalized reconstruction implants with promising features.


After those two milestones, surgical guides and porous implants, we kept collaborating with Materialise to imagine new applications. While working on the development of bone-borne cutting guides for orthognathic surgeries, we came up with the idea of inserting dental implants in the fibula flap at the very first stage of the operation. That resulted in the launch of a personalized solution combining drilling guides and personalized plates and implants in 2012. This is a solution we still use today on a daily practice in orthognathic surgeries.
Very rapidly after that, we applied this combined solution of drilling guides and personalized plates or porous implants to almost any possible location of the facial skeleton for orthognathic surgery, but also post-trauma deformity or any other kind of deformity.
What about the accuracy of these devices? Could you trust the results from the beginning?
The first case I operated using this combination of personalized drilling guides and implants was in July 2012, and I remember it as if it was yesterday. The procedure involved a maxillary osteotomy.
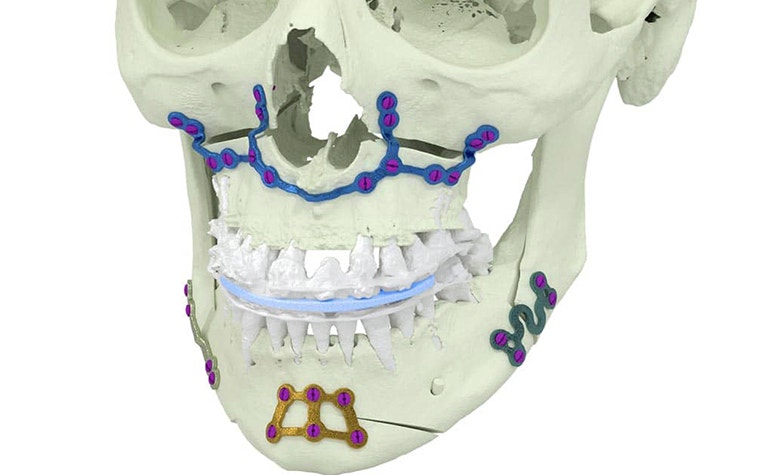

The result of this first case was already surprising, even before we could make a precise assessment of the accuracy. After a couple of cases, we started superimposing the post-operatory CT scan with the 3D planning and measuring the distances of the planning with the outcome. We were astonished to see how accurate the plan was to the outcome.
As the accuracy of the new personalized devices could be trusted from the beginning, what were the main challenges to develop this technology further?
Later we started working with Materialise to develop the same technology for the mandible. The challenge there was not really on the development of the devices but rather on the planning.
For the maxilla, the planning is straightforward because we start with one bone where nothing is moving, and we mobilize one segment of the bone and position it according to a fixed, stable part. The mandible moves. The joints between the mandible and the facial skeleton make the planning much more complicated as you must consider where this joint should be at the end of the surgery. Most pioneer surgeons in digital planning, including myself, did not fully understand this at the beginning. We were used to the conventional planning, and it was not obvious to digitally plan the repositioning of the condyles.
Is the use of 3D planning the most challenging part of using personalized devices?
Digital planning is way easier now. Back in 2012, I was doing all the planning myself. We had no clinical engineers trained in digital clinical planning at that time. I had to digitally adjust the occlusion just by looking on the screen, zooming in and out.
The planning is now much faster, systematic, and reliable. Many steps are now automated, and we have also developed a checklist that identifies and validates each step of the planning separately.
That helps a lot to make sure that every step is perfectly planned before going into the final validation.
Today, at least at Materialise, surgeons have a clinical engineer to guide them through all the steps. The clinical engineers will ask their approval for every key aspect of the planning, like the orientation of the head, the design of the osteotomies, and any other adjustment the surgeon would like to make in the planning.


Another significant achievement was the improvement of the CMF planning software itself. Materialise brought a lot of development, including the introduction of additional tools that help you to make almost any measurement possible and gives you the confidence to position all the bone segments in a perfectly symmetrical manner. Today we can even see the measurements changing in real-time while you are adjusting or displacing some bone segments.
What are the main advantages of taking a personalized approach?
It is essential to mention that in a broader context, every time you plan, you are taking a personalized approach. Personalization itself is not something new, but what has changed are the available tools for treatment and the possibility to adapt it to each patient.
As maxillo-facial surgeons, we have a long-standing habit of planning most of our treatments and surgeries, even for standard protocols. Preoperative planning helps us to make decisions beforehand and anticipate what we want to do during the surgery. Before, there was no way to visualize the shaping of a bone flap, for instance, and barely any guidance during surgery.
Now, when I see this digital model of the facial skeleton, the whole face, I can try multiple scenarios of how to position the bone segments before deciding on the ideal one. Digital planning is a real and customized training session before every surgery we perform.
In addition, you have the personalized devices to guide you to apply your planning during the surgery. We can focus on every other essential steps of the surgery instead of having to decide intraoperatively where are we going to position the bones, and that is very helpful.
Where do you draw the line to use personalized devices?
I opt for them as often as possible. I see an added value for basically every case. You can spare a lot of time during the surgery. For me, there is no debate about this.
In France, the health insurance does not reimburse personalized solutions, so the hospital takes on the cost. This is a significant cost for a hospital, so I need to justify why I am opting for these devices. I can perfectly demonstrate that we can save up to an hour and a half in the operating room for a free-flap surgery, for example. In the case of orthognathic and trauma surgeries, we would do something like two osteotomies in a day and now we can perform three to four surgeries in a day, in the same operating room.
Additionally, it is demonstrated that the repositioning of the bone is much more accurate with personalized devices. In CMF, whether it is a reconstruction or a functional surgery, those are not considered essential treatments. That means that it is challenging to justify the need for a revision surgery. So, it is crucial to go for optimal accuracy the first time, and personalized implants do present much better results in terms of accuracy.
Over the last few years, we’ve seen more and more personalized solutions on the market. What is essential to consider before choosing a solution?
I have been working with Materialise since 2005, and we have always had a robust research and development collaboration. Materialise is a real developer of technology instead of just adapting another solution to a portfolio.
What makes a difference in working with Materialise are the validation processes, including both the planning and the manufacturing of the devices. I know how serious they are about checking every point, and it is impressive to see all the effort put into making sure that the best quality is in everything. Materialise is also developing software, devices, process, so it is interesting to actively participate in this constant improvement process.

From my experience with other companies, for TMJ implants, for example, there are some excellent solutions available. The implants themselves are very nice and work well. However, the planning part and the preparation of the implant is not always so easy.
In the case of personalized solutions, the communication and the planning process are as important as the technical characteristics of the device.
Every guide, every implant has unique measurements, so you need to be able to rely on the company's commitment to achieve the most optimal results out of the planning and the designed implant.
What advice would you give to surgeons considering using personalized solutions?
In my lectures, I always remind the surgeons that personalized solutions are just a tool. This tool allows us to perform surgeries, including very complex ones, with excellent predictability and reliability as long as the surgeon stays in total control of every step of the surgery. Some younger surgeons may think they can perform procedures that exceed their skills because they are using personalized solutions. However, the success of a surgery still relies mainly on the surgeon’s skills, so you just should go for surgeries you are already comfortable performing.
In the case of surgeons who don’t feel confident to work in a digital environment, clinical engineers can help a lot to facilitate this transition. The exciting thing about digital planning is to see how your initial diagnosis and treatment plan often changes once you can visualize the 3D planning where you can virtually move skeleton pieces, jaws, etc.
My advice is to take as much time as needed for the first cases. Planning is faster in a digital environment than with conventional protocol, but this is only true after practice. Once you learn to use the digital tools, it will take you about 10 to 30 minutes on average to have your plan ready.
L-101480-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
