
INTERVIEW
Personalized Guides for Partial Knee Replacement: A Conversation with Zimmer Biomet
Materialise has long been at the forefront of personalized healthcare, leveraging game-changing technologies in surgical tools and planning. In the field of orthopaedic joint reconstruction, our personalized implants, guides, and planning software have allowed surgeons to build customized plans specific to a patient's anatomy and add more accuracy and predictability to their procedures.
One of our longtime partners in this field is Zimmer Biomet, a global leader in musculoskeletal healthcare. Founded in 1927, they are one of the largest manufacturers of orthopaedic reconstruction products globally and the market leaders in knee and hip replacement. They also offer various enabling technologies designed to support the use of their implants, providing comprehensive and end-to-end service offerings on the market.
Zimmer Biomet was an early pioneer in personalized medical solutions, with their first personalized instrument developed by Materialise in a strategic partnership and launched in 2009.
Now, with the launch of personalized knee guides for the Persona® Partial Knee implant last January, we spoke with Johan Hermans, Zimmer Biomet Associate Director for Personalized Solutions in EMEA. Johan was present for the first knee surgery using 3D-printed guides, and he told us about the history of the guides, what these new guides mean for both patients and surgeons, and what we can expect from personalized solutions in the years to come.
Our collaboration introduced 3D-printed guides into the OR in 2009. With more than 300,000 patients now treated, this product has proven the value of the personalized approach in orthopaedics. Can you tell us more about the pioneering role of Zimmer Biomet and Materialise in personalizing surgery?
When the Materialise guides came to the market, Zimmer and Biomet were still two separate companies. Both were working with Materialise as a strategic partner to develop technology in 3D planning and printing.
At the time we launched the guides, 3D printing was a new technology in the medical field. The printing of models had been used before; however, the introduction of the guides has brought the possibility to 3D plan the surgery and transfer this planning to the operating room (OR).
I still remember the first case, a surgery in Brussels — the surgeon was really impressed with how the guide fit the patient's anatomy. It was a real aha! moment.
Before this, the only thing that a surgeon could do was templating, which is more about defining the implant's size and is mostly only 2D.
So the shift from 2D to 3D was significant because it has allowed the surgeon to see the anatomy in 3D during planning. What kind of impact did this have on the surgery?
Surgeons using the new technology were impressed with the possibilities brought on by the virtual surgery. Many of them reported that the technology had helped to better understand how to reconstruct the knee and decide on each patient's best approach. This is the essence of personalized solutions — it is not just about specific instruments but about a holistic offering to allow the surgeon to customize the solution to each patient.
Other feedback we commonly received was that the 3D planning technology was useful in helping junior surgeons or registrars better understand how the procedure works.
Can you explain more about the value of using 3D planning and guides in knee surgery?
First, the technology helps the surgeon make a very detailed preoperative plan based on a 3D reconstruction of MRI or CT scans. This may help to avoid surprises during surgery.
Second, by using 3D planning, the optimal implant sizes for each patient can be assessed preoperatively. Having the correct sizes available upfront, combined with the guides transferring the preoperative plan, can enhance efficiency in the operating theater, as you need fewer instruments to perform the surgery. This, in turn, may shorten surgery time.
Finally, there may also be an effect on the OR setup time for each patient, and the number of instruments needed for cleaning and sterilization may be reduced. In a fully optimized setting, we can reduce the number of instrument trays from six to two and decrease OR time up to 16 minutes for each case.1 This may bring cost-efficiencies for the hospitals and provides us with the possibility, as an implant company, to optimize the stock of implants at the hospitals. For example, for our Persona Total Knee Implant, we offer hospitals a dedicated instrument set, called Green Line, which includes the guides. That set may allow hospitals to maximize benefits and increase efficiency in the OR.
Zimmer Biomet and Materialise are now launching 3D planning and guides for the Persona Partial Knee Implant, the first enabling technology available for this implant. Can you explain how this launch will benefit surgeons and patients?
It is critical for implant survival that the procedure is executed well. Assisting technology can make a big difference for surgeons.


In addition to the general advantages of guides, I see these specific benefits for partial knees; during the 3D planning, the surgeon can fine-tune the tibia implant's exact position and optimize implant coverage without creating overhang. This is critical to help avoid pain or discomfort for the patient post-surgery.
Next, the surgeon can adjust the femoral and tibial resections in the plan, considering the tibia insert thickness and the post-operative leg alignment he is aiming for. With partial knee surgery, the alignment mustn't be overcompensated, as this could potentially cause problems for the patient in the future.
Another unique feature is the indication of the required saw blade length on the surgical plan report. When using a calibrated saw blade, the surgeon can be more confident that the blade will go only as far as needed, reducing the risk of damaging soft tissues.
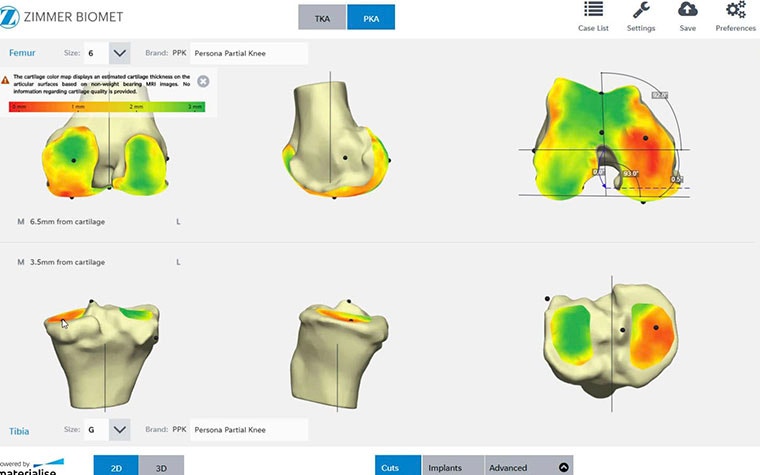
Finally, the surgeon can access a cartilage colormap during the planning phase to view the cartilage left in the different regions of the joint surface. To my understanding, Materialise is the only company offering this unique feature.


How is the market for partial knee surgery evolving? How do you see the adoption of planning and guides?
We see the trend toward partial knee replacement increasing. The partial knee market is growing three times faster than the total knee market. Since last year, national organizations like NICE in the UK, are actively recommending that patients who are elected for a partial knee should be offered a choice between the partial or total knee.
Data of patients treated with a partial knee implant report faster recovery, less pain, lower opioid use, lower complication rates, shorter length of stay, and fewer readmissions.2, 3, 4
Today, studies of optimal partial knee usage recommend that surgeons use a partial knee in at least 20% of their knee procedures. For surgeons who are new or infrequent users of partial knee replacement, the technology can play an important role in giving these surgeons the extra confidence they need to increase partial knee volumes. We believe that 3D planning and guides will play a significant role in helping this shift from total to partial knee for selected patients.
As a closing thought, where do you see the future of 3D planning and guides going, and what's their role in the personalization of surgery?
There is still a lot of potential to further personalize knee surgeries. What we see happening more and more now is that surgeons want to stay closer to the patient’s specific alignment. When surgeons want to personalize the alignment for their patients, it is even more essential to plan and reproduce that plan accurately. This can be achieved with knee guides or with other enabling technologies, such as Zimmer Biomet’s ROSA® robot or smart navigation, iASSIST, depending on the hospital environment.

Another important aspect is that surgical planning is evolving to become data-driven. By collecting more pre-, intra-, and post-op data and combining it with artificial intelligence, we expect surgery for every patient to become even more personalized, which may result in improved patient outcomes and reduced revision rates. So we are very happy with the knee guides we offer together to our customers and their patients, now also for our Persona Partial knee. And we definitely see a bright and personalized future ahead.
1 Kassab, S., Pietrzak, W. Intraoperative Benefits of Signature Personalized Patient Care in Total Knee Arthroplasty. White Paper. 2012.
2 Lombardi, A. et al. Is Recovery Faster for Mobile-bearing Unicompartmental than Total Knee Arthroplasty? Clinical Orthopedics and Related Research. 467:1450-57. 2009.
3 Amin A, et al. Unicompartmental or Total Knee Replacement? A Direct Comparative Study of Survivorship and Clinical Outcome at Five Years. JBJS Br. 2006; 88-B; Suppl 1, 100.
4 Deshmukh, RV, Scott, RD. Unicompartmental knee arthroplasty: long term results. Clinical Orthopedics and Related Research. 2001; 392:272278.
L-101795-01
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
