EXPERT INSIGHT
6 Questions to Ask Before Starting with 3D Printing in Your Hospital (Part 1)
Over the past 20 years, 3D printing has emerged as a disruptive technology in the healthcare field — it’s been used to create custom devices and instruments, plan complex medical procedures, and better train future medical professionals. As the accessibility to the technology increases, hospitals are beginning to adopt 3D printing programs within their own institutions, aiming to reduce lead times for 3D-printed models and build knowledge internally. But along with the tremendous potential of 3D printing, there are also significant challenges to its widespread adoption. Where should you start? Here are the questions you need to answer while you consider getting started with 3D printing in your hospital.
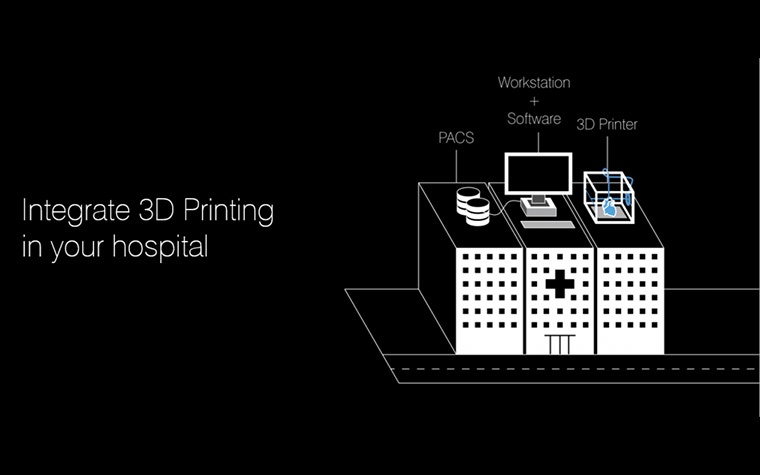

What is your ideal scale for the 3D printing program: departmental or institutional?
If your goal is to support a single medical discipline with 3D printing, the hardware and software necessary will be very different from those needed to provide a large-scale service institution-wide. The scale of the operation will impact not only the resources required but also the optimal workflow.
For example, an institution-wide 3D printing service could not function optimally without a software overview of the entire workflow, enabling your personnel to identify at all times what stage any particular project is at. On the other hand, your workflow will also look very different if you are building anatomical models to support congenital heart surgery rather than bone models for complex cranio-maxillofacial surgery.
What is the optimal imaging format for your 3D printing application?
Whether you are building anatomical models or personalized medical devices, great imaging is the precursor to accurate 3D models and an efficient process. CT or MRI? Contrast-enhanced or non-contrast? Which imaging modalities and protocols are needed? Each odelling application will have unique imaging requirements, so a close collaboration with your imaging departments is key.
It is also important to define the appropriate protocols as early as possible to avoid the need to re-scan a patient or to work with less-than-optimal imaging. In general terms, it is best to acquire high resolution, both spatial and temporal, images to achieve the best 3D printing results (thin-slice, gated imaging). Lean on the expertise of your radiologists to assist in optimal protocol definition or reach out to the industry for recommendations.
What software tools will you need throughout the workflow?
One aspect that tends to get overlooked is the appropriate processing of your medical imaging data for 3D printing. To optimize your workflow from DICOM imaging to the 3D printer, it is best to find a single software solution that addresses each step of the workflow. This will save you time and reduce the headaches and errors that can arise when linking steps between software programs licensed by different vendors. Considering that the results of your odelling will be used to supplement clinical decision-making, you must choose software tools that are cleared for medical use.
As a general rule, start first by fully understanding the needs of the clinician for a specific use case. Will the model be used as a pre-surgical planning tool? Or for education or training? Understand the necessary anatomy and additional landmarks needed in the model to work most efficiently. By fully understanding the scope of the project from the beginning, it will ensure a useful model for the surgeon, save time in the segmentation/modeling process, and often lead to a faster build using less material.
Image processing
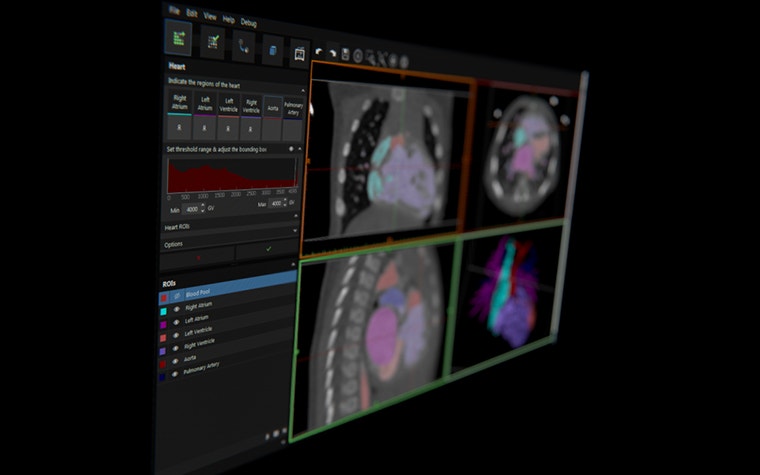
Even if you are accustomed to preparing CT, MRI, or 3D ultrasound data for traditional image processing and 3D volume rendering techniques, the considerations you have to keep in mind while preparing for 3D printing are very different. The one tool that you will need to bridge this gap is an appropriate 3D medical imaging software tool that has a strong combination of automated and manual segmentation functionality.
The next steps in your workflow are all based on this segmentation, so it’s of crucial importance. Often the cases that will benefit most from 3D printing are also the most complex in terms of anatomical anomalies. This can challenge even the most sophisticated segmentation algorithms, so also find a tool that enables efficient manual intervention during segmentation when necessary. In addition, it is useful to have a tool that can reconstruct and render your STL files within the software instead of a simple STL export option. This gives you the advantage of seeing and verifying what you have created prior to 3D printing.

In the follow-up blog post, we’ll further describe how you can create an accurate file for 3D printing (including modeling, verification and labeling, and file fixing). Or watch the webinar recording about implementing 3D printing in your hospital to learn more.
This blog is based on an article first published on auntminnie.com
Share on:
You might also like
Never miss a story like this. Get curated content delivered straight to your inbox.
